The aim is to study the sleep duration and the 24-h sleep distribution pattern in children under 2 years old from two different areas of Spain, as well as to determine the prevalence of abnormal sleep duration and the influence of age on this prevalence, and compare them with the already published data.
Materials and methodsAn observational, descriptive and cross-sectional study on children from two health centers: one in Castilla y León and the other in Asturias. Their parents completed the Brief Infant Sleep Questionnaire (BISQ). Daytime and nighttime sleep durations were assessed, with percentiles being used to evaluate the results. Two groups were created: one according to the age (children under or above 6 months), and the other according to the area.
ResultsA total of 125 children were studied (73 males). The nighttime sleep duration increased from 8.28±2.06h to 10.43±1.21h (P=.0001) and the daytime sleep decreased from 4.61±2.66 to 1.96±0.79h (P=.0001) for children under 6 months and above 6 months, respectively. The children from Castilla y León slept more during daytime than those from Asturias (3.91±2.67 vs. 3.00±2.09h, P=.041). Nineteen children had a total sleep duration below the 2nd percentile. A sleep duration below normal percentiles was observed in children under 6 months (14/72 vs. 5/53, P=.006).
ConclusionsAs children grow older, they substitute daytime sleep for nighttime sleep. Approximately 15% of the children under 2 years-old may have changes in sleep duration, and is more common in children under 6 months.
Conocer si en nuestro medio la duración del sueño y el patrón de distribución del sueño a lo largo del día en <2 años son similares a los publicados. Obtener información sobre la prevalencia de las alteraciones de la duración del sueño y sobre la influencia de la edad en dicha prevalencia.
Material y métodosEstudio observacional, descriptivo, transversal realizado en niños <2 años de 3 centros de salud de León y Asturias. Mediante la cumplimentación por sus padres del cuestionario de sueño Brief Infant Sleep Questionnaire (BISQ) se analizó la duración del sueño. Para evaluar alteraciones en la duración del sueño se utilizaron percentiles de duración del sueño. Los resultados fueron valorados en el conjunto de niños encuestados y en los 2 grupos creados para su comparación (niños>y<6 meses) (niños de León y Asturias).
ResultadosSe incluyeron 125 niños <2 años (73 varones). El sueño nocturno aumentó desde 8,28±2,06h en <6 meses hasta 10,43±1,21 en >6 meses (p=0,0001), disminuyendo el sueño diurno desde 4,61±2,66 a 1,96±0,79h (p=0,0001). Los niños leoneses duermen durante el día más horas que los asturianos (3,91±2,67 vs 3,00±2,09h, p=0,041). Diecinueve niños tuvieron una duración total de sueño<percentil 2, siendo más frecuente en niños <6 meses (14/72 vs 5/53, p=0,006).
ConclusionesLos niños sustituyen el sueño diurno por el sueño nocturno según van creciendo. Aproximadamente el 15% de niños <2 años podría tener trastornos en la duración del sueño, siendo este hallazgo más frecuente en <6 meses.
Physiological functions that are essential to the correct psychological and physical functioning of individuals take place during sleep.1 This is particularly important in the early months of life. During this period, children develop the ability to sleep for long intervals of time predominantly at night, approaching the sleeping patterns of adults2; regular sleep–wake patterns are established, which are good indicators of healthy child development3; and if problems in sleep consolidation arise, they tend to persist throughout childhood.4
It is known that the total duration of sleep decreases with age and that significant changes take place in the first months of life.5 The number of hours that a child needs to sleep is not exact, as each child, just as it happens with adults, has specific individual sleep requirements. It is believed that the hours of sleep needed are those that allow the child to function well in his or her daytime activity.6 On the other hand, we know that there are cultural and geographical differences in regards to total sleep duration, night wakings, bedtimes, and naps.7,8
Sleep disorders have a high prevalence and interfere with the normal sleep pattern, affecting both its duration and quality, or with the sleep–wake cycle regulation.4,5 Sleep duration percentiles are a very useful tool to detect sleep problems that affect sleep duration, and allow making comparisons throughout childhood.3
The purpose of this study was to learn whether sleep duration in children younger than 2 years in our region and the physiological changes that take place in the pattern of sleep distribution during the day in this period of life are similar to those reported in the literature, and whether they are influenced by the region of origin. We also used percentiles to collect data on the prevalence of sleep duration disturbances in the children under study, and on the influence of age and geographical location in this prevalence.
Materials and methodsWe performed a cross-sectional, descriptive observational study on sleep duration between May and June of 2012 in children younger than 2 years that came to 3 healthcare centres of León and Asturias (La Condesa and Eras de Renueva in León, and Mieres Sur in Asturias) for their well-child checkups.
Once the well-child checkup was finished, and having informed the parents of the aim of the study and obtained their informed consent, the parents or legal guardians of the child answered the following questions concerning sleep duration, which had been taken from the Brief Infant Sleep Questionnaire (BISQ)4:
- -
How much time does your child spend sleeping during the night (starting at 9 in the evening)? (Hours and minutes).
- -
How much time does your child spend sleeping during the day (starting at a 9 in the morning)? (Hours and minutes).
- -
How much time does your child spend awake during the night (from 12 at night to 6 in the morning)? (Hours and minutes).
- -
How many times does your child wake up during the night?
- -
How long does it take your baby to fall asleep in the evening (from the time your child is put to bed)? (Hours and minutes).
- -
What time does your child usually fall asleep at night (first sleep)? (Hours and minutes).
To assess the presence of sleep duration disturbances we used the percentiles for total sleep duration published by Iglowstein et al.9 We considered that sleep duration was shortened if it fell below the second percentile (P2) for the child's age.4,6
The results obtained from the sleep questionnaire were analysed for the entire group of children, and for the 2 groups created for their comparison according to age (children younger and older than 6 months) and region of origin (León and Asturias).
We performed a descriptive statistical analysis of the different quantitative variables under study (range, interval, mean, and standard deviation). We have expressed qualitative variables as percentages and frequencies. We compared quantitative variables between independent samples using Student's t test, assuming that the variables had a normal distribution. Qualitative variables were compared between groups by means of the chi-squared test. Correlations between quantitative variables were analysed using the Pearson correlation coefficient. The level of statistical significance was set at P<.05 (alpha level of 5%) for all tests.
ResultsThe study included a total of 125 children younger than 2 years, 73 of whom were male (58.4%) and 52 female (41.6%). Their mean age was 8.39±6.99 months (range, 1–24 months); 72 (19.4%) were younger than 6 months, and 53 (84.8%) older than 6 months. Seventy-seven children (53.6%) were selected from the 2 healthcare centres in León, while fifty-eight were selected from the healthcare centre in Asturias (Mieres Sur).
Table 1 presents the data on daytime and nighttime sleep duration, time spent awake at night, and sleep onset latency for the children in this series, as a whole and separated by age group (younger and older than 6 months).
Comparison of sleep characteristics by age group.
| Total series | Children <6 months | Children >6 months | P | |
|---|---|---|---|---|
| Nighttime sleep (hours) | 9.20±2.05 | 8.28±2.06 | 10.43±1.21 | .0001 |
| Daytime sleep (hours) | 3.48±2.46 | 4.61±2.66 | 1.96±0.79 | .0001 |
| Nighttime wakefulness (minutes) | 33.49±60.81 | 56.47±73.96 | 4.90±8.00 | .006 |
| Sleep latency (minutes) | 23.10±29.34 | 23.78±34.15 | 22.17±21.40 | .76 |
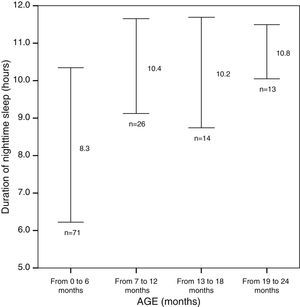
Although in our series we did not find differences between the two age groups in the total sleep duration (12.89±2.41h in children younger than 6 months vs. 12.39±1.01h in older children; P=.88), children younger than 6 months spent less time sleeping at night and more sleeping during the day, and were awake longer at night (Fig. 1). We did not find any differences in sleep onset latency between the two age groups (P=.76).
The number of night wakings was similar in both groups, with children younger than 6 months waking a mean of 1.61±1.15 times and children older than 6 months 1.23±1.33 times (P=.09).
The sleep onset time was similar in both age groups (21.01±4.86h in children younger than 6 months and 21.87±0.87h in children older than 6 months; P=.20).
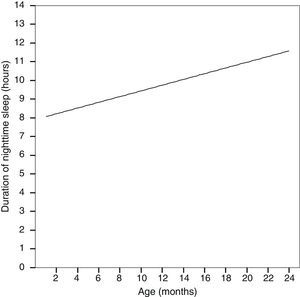
Age showed a strong direct correlation with the duration of nighttime sleep (Pearson's r=0.524; P=.0001) (Fig. 2) and an inverse correlation with the total hours of daytime sleep (Pearson correlation coefficient, −0.552; P=.0001).
Age was negatively correlated with the time spent awake at night (Pearson's r=−0.425; P=.0001). The correlations between age and sleep latency, the number of night wakings, and sleep onset time were not statistically significant.
Table 2 shows the data on daytime and nighttime sleep duration, time spent awake at night, and sleep latency for the children in our case series separated by geographical location (León and Asturias).
Comparison of sleep characteristics by region of origin.
| Total series | León | Asturias | P | |
|---|---|---|---|---|
| Nighttime sleep (hours) | 9.20±2.05 | 9.15±2.06 | 9.26±2.04 | .65 |
| Daytime sleep (hours) | 3.48±2.46 | 3.91±2.67 | 3.00±2.09 | .041 |
| Nighttime wakefulness (minutes) | 33.49±60.81 | 35.46±56.19 | 30.42±68.09 | .62 |
| Sleep latency (minutes) | 23.10±29.34 | 23.61±31.73 | 22.50±26.57 | .84 |
Children from León slept more hours during the day than children from Asturias (3.91±2.67h vs. 3.00±2.09h; P=.041). We found no differences between the two groups in the duration of nighttime sleep, the time spent awake during the night, and the sleep latency.
We found no differences between children from the different geographical regions in the number of night wakings (1.56±1.20 times vs. 1.31±1.28 times; P=.10) or the sleep onset time (21.09±4.35h vs. 21.71±2.90h; P=.19).
Of the 125 children younger than 2 years included in this study, 19 had a total sleep duration below the P2 for their age. Sleep durations below the normal percentile for the age were significantly more frequent in infants younger than 6 months (14/72 vs. 5/53; P=.006). In our study, the total duration of sleep in hours was above the 98th percentile in only one child.
Of the 19 children whose sleep duration was below the P2, 10/58 came from Asturias and 9/67 from León (P=.99). The child whose sleep duration was above the 98th percentile came from León.
DiscussionSleep is an essential activity that needs an adequate duration and quality for individuals to maintain their psychological and physical wellbeing.1 The American Academy of Sleep Medicine established the International Classification of Sleep Disorders in 2005 to determine what could be considered normal or pathological in sleep during childhood. There are about 70 sleep disorders.10
However, the number of hours that a child needs to sleep is not exact, as each child, as happens with adults, has individual sleep requirements, although it is generally considered that the necessary number of hours of sleep are those that allow the child to function well in his or her daily activities.6
Sleep disturbances impact the total sleep duration and interfere with the adequate consolidation of nighttime sleep. Several longitudinal studies have documented the persistence of sleep disturbances in 30–40% of affected children at age 36 months.4 In 1992, Pollock reported that children that have sleep problems in the first six months of life are three times as likely to continue having problems at 5 years of age and twice as likely to have sleep problems at 10 years of age.11
Despite the high prevalence of sleep problems and their comorbidities, they are not properly screened for in paediatric practise. Screening for sleep problems requires a detailed history taking, a full physical examination, and the use of supporting tools such as sleep percentile tables, sleep diaries, home videos, sleep problem screening questionnaires and diagnostic tests. The use of sleep percentiles and sleep disorder screening questionnaires is of particular interest, as they can help quickly detect problems in primary care practises.
There are many questionnaires that assess sleep habits.12,13 We chose the BISQ for our study because it is a quick means to detect abnormalities in the total duration of sleep, the distribution of sleep hours between night and day, and the quality of sleep measured in terms of the number of wakings and the sleep latency. Completing the questionnaire takes only 5–10min, which is very important, as one of the main reasons why a proper screening for sleep disorders is not performed is the little time available in primary care visits.1
We chose the population of children aged up to 2 years because this is the period of life during which the most meaningful changes in sleep take place. Sleep is different in a newborn than in an infant, with wake–sleep cycles that recur several times a day (ultradian rhythms). Starting at 4–6 months of age, this wake–sleep cycle starts to change in a progressive and shifting manner through the first years of life into a single 24h cycle (circadian rhythm).11 It takes children between 5 and 6 months to achieve a regular rhythm in their activities, including sleep, partly because it is the time required for the maturation of the suprachiasmatic nucleus of the hypothalamus responsible for regulating circadian rhythms.3 During this time, most children develop the capacity to sleep for long periods of time with a predominance of nighttime sleep, approaching adult sleeping patterns.5
Total sleep duration decreases with age, which results especially from a reduction in the hours of daytime sleep and from nighttime sleep consolidation.5 Although we did not observe a decrease in the total duration of sleep in the older children in our sample, our results did show swift changes in sleep distribution patterns during the first six months of life, with hours of daytime sleep getting replaced by hours of nocturnal sleep, consistent with what has been reported in the literature.2
The literature also describes that nighttime sleep fragmentation decreases as the number of night wakings goes down from birth to 2 years of life.14 The consolidation of nighttime sleep is characterised not only by fewer night wakings, but also by the decreased duration of these wakings and by the increased duration of the longest continuous episode of sleep.15 While in our study the number of wakings was greater in infants younger than 6 months than in older children, this difference was not statistically significant. However, the fact that younger children stayed awake longer is consistent with the greater sleep fragmentation found in this period of life. It is worth noting that in our series the number of night wakings in infants younger than 6 months was only slightly greater than 1.5 per night, while the literature describes that over half of the children in this age group wake up at least 3 times a night.16,17 This may be due to the fact that nighttime sleep is influenced mostly by cultural or ecological factors, as opposed to daytime sleep, which depends mostly on biological factors.18
Unlike what we observed in our results, several studies show that sleep latency shortens as age increases. The time it takes children to fall asleep gradually decreases over the second half of the first year of life.14 Cultural factors may also account for this difference.
Bedtimes do not vary by age group in children from Asian countries, while in Caucasian children they become earlier from birth until six months of age, after which they remain relatively unchanged.8 Although in our study children older than 6 months seemed to go to sleep a little later than younger children, this difference was not statistically significant.
Sleep duration also depends on geographical and ethnic factors. Children from Asian countries sleep fewer hours during the night and fewer total hours, and go to bed and get up at later times.7,19 In our study, we only observed a difference between children from the two geographical areas in their daytime sleep duration, which was nearly 1h longer in children from León. Asturias and León are neighbouring regions with hardly any geographical and ethnic differences, but with slightly different socioeconomic and cultural characteristics that may account for this finding.
There are no exact data on the sleep requirements of different children, and it is common for clinicians to meet parents that are worried that their children are not sleeping enough hours for their age and that overestimate the sleep requirements of children. Published studies diverge up to 3h in the total sleep duration of their populations.
Few publications present specific values for normal sleep duration in each age group. The study done by Iglowstein et al. in 2003 was the first published to include sleep duration percentile curves for children ranging from infancy to adolescence.9 In addition to describing the increase in the hours of nighttime sleep that takes place with age, an interesting finding in this study was the great variability in the total hours of sleep that could be considered normal. For instance, in the period ranging from 3 to 11 months of age, the second percentile for the total hours of sleep (the lower limit of normal) ranges between 9 and 10h, and the 98th percentile (the upper limit of normal) nears 19h. These large differences point at a considerable interindividual variability in sleep requirements or opportunities that reflect the influence of biological or environmental factors.17
It is worth noting that nearly 20% of children younger than 6 months in our study had total sleep durations below what is considered normal. This was observed in children from both León and Asturias, and while the relevance of this fact would be hard to assess, we believe it should not be overlooked. Future studies should be done to confirm this finding, and should it be confirmed, to assess whether the percentile tables currently used are appropriate for all populations.
To conclude, we want to mention that this study confirms that questionnaires that screen for sleep problems and percentile tables are useful tools for primary care paediatricians, and provide relevant information on factors related to sleep duration.
Conflicts of interestThe authors have no conflicts of interest to declare.
Please cite this article as: Fernández Miaja M, Rodríguez Fernández C, Fernández Pérez ML, Mata Zubillaga D, Miaja Quiñones J, Rodríguez Fernández LM. Cuantificación del sueño y presencia de alteraciones en la duración del sueño en niños menores de 2 años. An Pediatr (Barc). 2015;82:89–94.