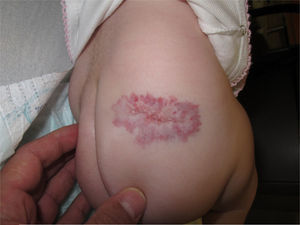
Ulceration is the most common complication of infantile haemangioma, occurring in 15.8% of cases, usually in the proliferative phase. It can be managed in several ways. We present our experience in the treatment of ulcerated haemangioma with the combination of pulsed dye laser and propranolol.
Material and methodsA retrospective observational study was conducted on patients with ulcerated infantile haemangioma treated with pulsed dye laser in association with propranolol. The study included 7 patients, 3 cases in the labial area and 4 cases in the nappy area. A review was also performed on a historical cohort of 5 children with ulcerated haemangiomas with the same features, but treated only with propranolol, topical agents and occlusive dressings.
ResultsThe median size of the ulcer was 1.0cm, with mean time from onset to treatment of 2 weeks. Pain and bleeding was present in all patients. After 2 weeks of combined propranolol and laser treatment, all lesions healed. The pain disappeared after the first laser session. Patients with ulcerative haemangioma in the labial area obtained a better response than patients with haemangioma in the nappy area. The cohort of patients treated with propranolol required a mean healing time of 5.2 weeks, with the addition of an occlusive dressing with ointment.
ConclusionsWe believe that our results suggest that combined treatment, laser and propranolol has synergistic effects that accelerate the healing of ulcerated haemangioma, as observed in our patients. Further studies with larger numbers of patients are needed to confirm this finding.
La ulceración se trata de la complicación más frecuente de los hemangiomas infantiles, produciéndose en el 15,8% de los mismos, habitualmente en el apogeo de la fase proliferativa. Existen múltiples herramientas terapéuticas para el manejo de los hemangiomas ulcerados, sin que se haya demostrado una mayor eficacia de ninguna de ellas. Presentamos nuestra experiencia en el tratamiento con láser de colorante pulsado asociado a propranolol en los hemangiomas infantiles ulcerados.
Material y métodosRealizamos un estudio observacional retrospectivo de pacientes con hemangioma infantil ulcerado que recibieron tratamiento con láser de colorante pulsado asociado a propranolol. Estudiamos 7 pacientes; 3 con hemangiomas en la zona labial y 4 en la zona del pañal. Asimismo, revisamos una cohorte de 5 niños con hemangiomas ulcerados de similares características que solo recibieron tratamiento con propranolol, curas tópicas y vendaje oclusivo.
ResultadosEl tamaño medio de las úlceras fue de 1cm, con un tiempo medio de evolución previo al tratamiento de 2 semanas. En todos los casos había dolor y sangrado. Tras 2 semanas de tratamiento combinado con propranolol y láser, todas las úlceras se habían curado. El dolor desaparece tras la primera sesión de láser. Los pacientes con hemangioma ulcerado en la zona labial presentaron mejor respuesta que aquellos que lo presentaban en la zona del pañal. La cohorte de pacientes tratados únicamente con propranolol, curas tópicas y vendaje oclusivo precisaron un tiempo medio para la curación de 5,2 semanas.
ConclusionesNuestros resultados evidencian que el tratamiento combinado de láser de colorante pulsado y propranolol presenta un efecto sinérgico, acelerando la curación de los hemangiomas ulcerados. Se necesitarían más estudios, con un mayor número de pacientes, para confirmar estos datos.
Infantile haemangioma is the most frequent form of benign neoplasm during childhood. It is rarely present at the time of birth, and is characterised by a rapid proliferative phase, followed by a slow and progressive regression, which can last up to 5 or 7 years before complete resolution. The development of these tumours is usually benign. However, in some patients, they may present complications, including haemangioma ulceration. This occurs in approximately 15% of cases.1–4 When ulceration occurs, it seems to be more frequent in larger haemangiomas, of mixed type and segmental distribution, located in the lower lip, the neck and the perianal area. Early treatment to prevent pain and other complications is essential.5–7 Ulceration of the tumours occurs at a mean age of 4 months, at the peak of the proliferative phase, and may cause feeding and child care difficulties, depending on its location.
Bleeding associated with ulceration appears in 41% of cases, but is often clinically insignificant. Infection occurs in 16%7 of cases. Successful treatment of these tumours is usually complicated.4,7
Since 2008, when propranolol was first described in the treatment of infantile haemangioma, the prognosis for these tumours has changed drastically.5–12 When the ulcer appears, monotherapy or combination therapy with topical antibiotic creams, such as mupirocin, alcohol-based dyes such as eosin 2%,13 topical corticosteroids,14 as well as occlusive dressings with silver or colloids have been used. Even so, response to these treatments in the areas previously described is very limited. Other beta-blockers, such as topical timolol,15 have been used for treatment with similar results.
Laser therapy has also been described in the treatment of both haemangioma and ulcerated haemangioma.16–19
We present 7 cases of ulcerated haemangiomas treated with oral propranolol in combination with pulsed dye laser, with a rapid resolution of ulceration.
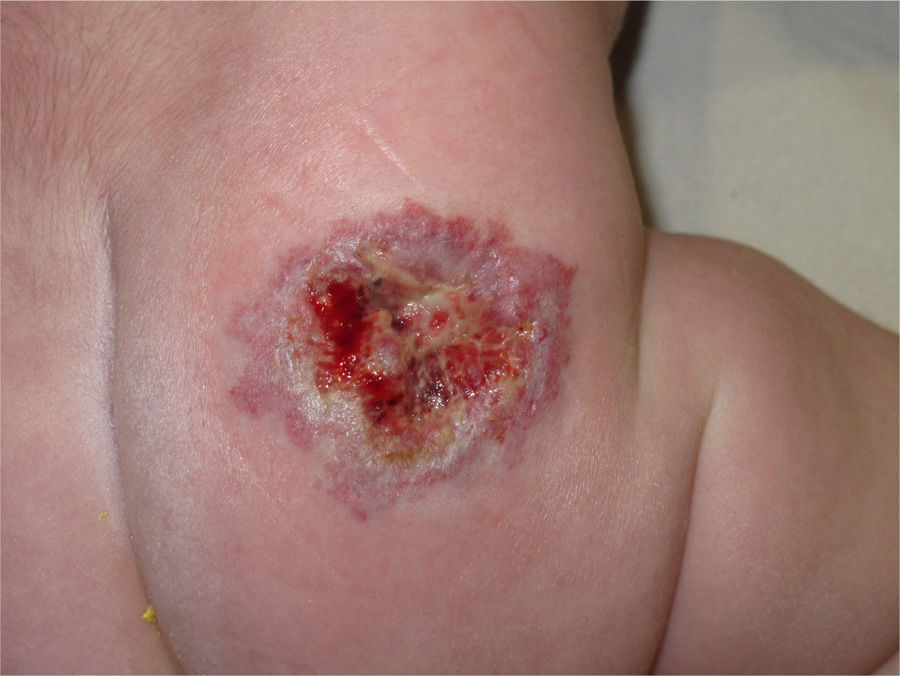
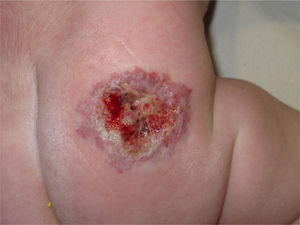
Material and methodsWe present a retrospective study of 7 cases of ulcerated infantile haemangiomas, 3 in the labial area and 4 in the nappy area. The average size of the ulcers was 1cm (±0.4) with a pre-treatment evolution of 2 weeks. All ulcers showed full thickness tissue loss without exposing tissue or muscle, with slough present in some cases, consistent with stage iii of the International Pressure Ulcer Classification System of the European Pressure Ulcer Advisory Panel.
All patients had pain and bleeding. After obtaining the signed informed consent of the legal representatives, off-label treatment was initiated with oral propranolol at a dose of 1mg/kg/24h, divided into 2 doses. For all patients, we added topical treatment with mupirocin in the ulcer area to prevent bacterial contamination of the wound and to stimulate healing. An occlusive dressing was applied to prevent bleeding and reduce the pain. Patients were checked weekly. After the first week of treatment with propranolol, the haemangioma improved in all patients, with changes in consistency and colouration, from intense red to duller tones. Accordingly, the propranolol dose was maintained unchanged. In spite of this, neither the ulcers nor the pain improved, causing the patients significant discomfort during feeding or nappy-changing, depending on the location of the haemangioma.
After 2 weeks of evolution, parents were offered laser treatment with pulsed dye laser (Cynergy™, Cynosure, Boston, MA, USA) with spot size of 7mm, 7 to 9J/cm2 and 0.5–2mseg pulses as a coadjuvant to oral propranolol. The procedure was performed under topical anaesthesia with lidocaine cream.
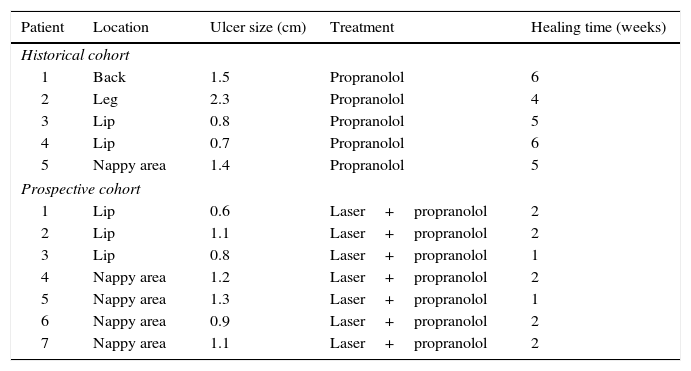
A historical cohort of 5 patients with ulcerated haemangiomas of similar characteristics treated with propranolol and topical mupirocin was also reviewed. In this group, mean time to complete resolution of the ulcer was 5.2 weeks (Table 1.)
Difference between both cohorts.
| Patient | Location | Ulcer size (cm) | Treatment | Healing time (weeks) |
|---|---|---|---|---|
| Historical cohort | ||||
| 1 | Back | 1.5 | Propranolol | 6 |
| 2 | Leg | 2.3 | Propranolol | 4 |
| 3 | Lip | 0.8 | Propranolol | 5 |
| 4 | Lip | 0.7 | Propranolol | 6 |
| 5 | Nappy area | 1.4 | Propranolol | 5 |
| Prospective cohort | ||||
| 1 | Lip | 0.6 | Laser+propranolol | 2 |
| 2 | Lip | 1.1 | Laser+propranolol | 2 |
| 3 | Lip | 0.8 | Laser+propranolol | 1 |
| 4 | Nappy area | 1.2 | Laser+propranolol | 2 |
| 5 | Nappy area | 1.3 | Laser+propranolol | 1 |
| 6 | Nappy area | 0.9 | Laser+propranolol | 2 |
| 7 | Nappy area | 1.1 | Laser+propranolol | 2 |
No statistically significant differences were observed in ulcer size between groups (p>0.05.)
ResultsIn all patients treated with laser and propranolol, pain disappeared immediately after the first laser session. There was no bleeding during or after the laser session. Improvement was evident in the first follow-up, one week after the laser session.
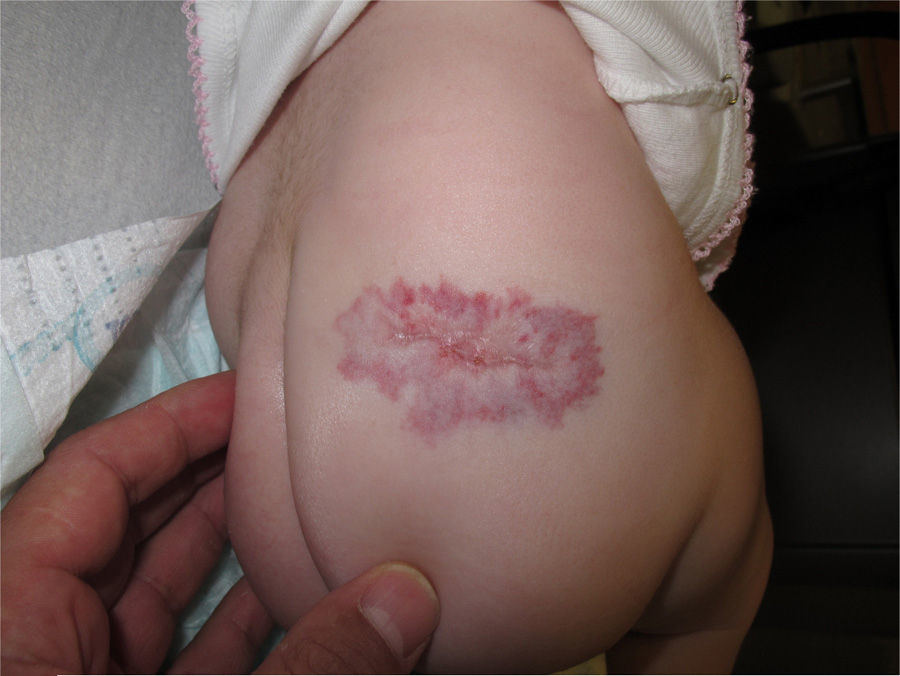
After an average of 1.7 weeks of combined laser and propranolol therapy, all ulcers in all patients had healed (Figs. 1 and 2). Patients with ulcerated haemangioma in the labial area showed a better response to treatment than those with ulcerated haemangioma in the nappy area, with a mean of 1 vs. 2 laser sessions, respectively, before complete resolution, although this difference was not statistically significant (p>0.05.)
No recurrence of ulceration was observed after a mean follow-up of 6 months.
In the historical cohort of patients treated only with propranolol, all patients required analgesic treatment until complete healing of the ulcer, as well as the application of topical mupirocin and occlusive dressing. This was not possible in all locations. The average time to complete resolution was 5.2 weeks. The haemangioma also presented improvement in parallel with the ulcer.
Data from both cohorts were compared using the Mann–Whitney test, and statistically significant differences in time to complete resolution were observed between treatments (p>0.05).
DiscussionUlcer formation is the main complication of infantile haemangiomas, and may occur in 15% of patients.7 An ulcerated haemangioma in the perioral area causes feeding difficulties, pain and bleeding, plus the risk of permanent aesthetic sequelae. Because of their location on skin that is often moist and in constant contact with the pacifier or the bottle during feeding, these ulcers do not heal easily. In some cases, friction may be the cause of pain and bleeding.7
In the nappy area, an ulcerated haemangioma causes significant problems, since pressure on the lesion in the supine position will cause pain, and the presence of faeces in this area undermines efforts to keep the wound clean.7
The use of oral propranolol for the treatment of ulcerated haemangioma has been described in multiple publications,5–12 although the response rate is limited.7 When comparing the healing time in our series of patients treated with propranolol and pulsed dye laser with the historical series of patients treated only with propranolol, we observed that better results were obtained with the combined treatment, with a statistically significant difference (p>0.05). This shows that adjuvant laser therapy greatly benefits clinical outcomes in this type of ulcer.20
The use of other types of lasers in the treatment of ulcerated haemangioma has been described, including argon laser, Nd:YAG, pulsed dye laser or pulsed light systems.16–21 The laser most frequently used in these patients is the pulsed dye laser, and most authors recommend its use in the care of ulcerated haemangiomas for pain control and ulceration improvement.
Recently, the use of propranolol associated with pulsed dye laser has been described for the treatment of uncomplicated haemangiomas.20 In this study, the authors conclude that segmental haemangiomas at the facial level treated with this combination therapy gave greater clinical improvement and faster and more noticeable lightening of the lesion colour than propranolol alone.
Our findings suggest that the synergistic effect of propranolol and laser treatment is more beneficial in the treatment of ulcerated haemangiomas than propranolol alone. Further studies in larger series of patients are needed to confirm this finding.
Conflict of interestThe authors declare that there are no conflicts of interest.
Please cite this article as: Rodríguez-Ruiz M, Tellado MG, del Pozo Losada J. Combinación de propranolol oral y láser de colorante pulsado en el tratamiento de los hemangiomas infantiles ulcerados. An Pediatr (Barc). 2016;84:92–96.