Breakfast is considered the most important meal of the day in a balanced diet. Skipping breakfast has been associated with overweight. This study aimed to describe overweight and obesity among secondary school students in Barcelona and to analyse their association with eating habits and sedentary behaviours.
Material and methodsA cross-sectional study was performed in 2008 on a representative sample of secondary school students in Barcelona (Spain). Overweight and obesity were defined using body mass index (BMI), which was calculated from objective measurements. The prevalences of overweight and obesity were determined, and their association with eating habits, sedentary behaviours, and physical activity was analysed using logistic regression models.
ResultsA total of 3089 students were analysed (52% girls). The prevalence of overweight was 26.1% in boys (6.2% obese) and 20.6% in girls (3.7% obese). In both sexes, overweight was associated with being younger, having breakfast less often, being on a diet, and with a lower frequency of unhealthy food intake. Being on a diet and a lower unhealthy food intake were related to obesity in both sexes. Among boys, obesity was also associated with sedentary behaviours.
ConclusionsThe results show that overweight and obesity are a serious public health problem and confirm the importance of breakfast to prevent overweight. Moreover, these results allow us to expand our knowledge on the factors associated with overweight and obesity in order to improve current school preventive programs.
El desayuno representa la ingesta más importante de una alimentación equilibrada y su supresión se asocia al sobrepeso. El objetivo del estudio es estimar la prevalencia de sobrepeso y obesidad en adolescentes de Barcelona y analizar su asociación con hábitos alimentarios inadecuados y conductas sedentarias.
Material y métodosEstudio transversal realizado en 2008 a una muestra representativa de estudiantes de secundaria de Barcelona. Se definió sobrepeso y obesidad en base al índice de masa corporal (IMC) a partir de medidas objetivas. Se determinó la prevalencia de sobrepeso y obesidad y se analizó su asociación con hábitos alimentarios, actividades sedentarias y actividad física mediante modelos de regresión logística.
ResultadosSe analizaron 3.089 escolares (52% chicas). La prevalencia de exceso de peso fue del 26,1% en chicos (6,2% obesidad) y del 20,6% en chicas (3,7% obesidad). En ambos sexos, el sobrepeso se asoció a una menor edad, menor frecuencia de desayunar, estar realizando una dieta para adelgazar y menor ingesta de alimentos menos saludables. Realizar dieta para adelgazar y una menor ingesta de alimentos menos saludables también se asociaron a la obesidad en ambos sexos. En chicos, además, la obesidad se asoció positivamente al sedentarismo.
ConclusionesLos resultados reflejan la magnitud del sobrepeso y la obesidad como problema de salud pública y confirman la necesidad de la toma de desayuno para prevenir el exceso de peso. Además, permiten ampliar el conocimiento sobre los factores asociados al sobrepeso y obesidad para mejorar los programas de promoción de la salud en escolares ya existentes.
Childhood obesity has been defined as the XXI century epidemic by the World Health Organization (WHO),1,2 and it is currently one of the main public health challenges in developed countries. In the United States, the prevalence of obesity in 2008 was 20% in boys and girls 6–11 years of age and 18% in youths 12–19 years of age, percentages three times as high as those observed in 1980.3 In 2001 in Spain, the prevalence of overweight in adolescents 13–18 years of age was 20% in males and 16% in females. This same study found a prevalence of obesity of 5.7 and 3.1%, respectively.4
Although obesity is a multifactorial disorder, social determinants and lifestyle play very significant roles. Low socioeconomic level,5 male sex6,7 and parental obesity have been identified as influential factors. On the other hand, an unhealthy diet, skipping breakfast or inadequate intake at breakfast,8–12 and sedentarism6 have been identified as lifestyles associated with obesity in childhood and adolescence.8–12
Breakfast should account for 25% of the total daily energy intake. An inadequate breakfast is usually compensated with greater intakes between meals or a greater percentage of the total daily energy intake in the remaining meals. Thus, an unbalanced energy intake through the day could lead to weight gain. Furthermore, the consumption of fruits, legumes, greens and vegetables has declined, while consumption of baked goods, sweets and snacks has increased, especially among adolescents with greater body mass index (BMI).8,10,11,13 On the other hand, the literature shows that the amount of screen time (television, computer or console) has increased among youth, which may contribute to a decrease in physical activity, which has a demonstrated dose–response association with overweight and obesity.6,11,13,14
In 1997, the WHO defined obesity in individuals older than 18 years as a BMI higher than or equal to 30kg/m2, and overweight as a BMI between 25 and 30kg/m2.1 However, it is not possible to establish set BMI cutoffs for excess weight (overweight and obesity) in children and adolescents, as at these ages they are going through a period of individual growth and development with patterns of fat deposition that vary depending on age, sex and pubertal development. Thus, valid estimates of excess weight in childhood and adolescence are made with growth charts with dynamic values adjusted for age and sex. While different methods to determine overweight and obesity in these age groups have been proposed, currently there is no universally accepted standard.15 In Spain, the charts traditionally used in health care settings are those proposed by Orbegozo et al.,16 while the cut-off points most commonly used in research have been those defined by Cole et al.,17 which are based on the populations of several countries representative of the global population and allow for comparisons between studies.
Although the association between eating habits and obesity in children has been shown in several studies,11 few of them have investigated the adolescent population in Spain.2,8,11 The aim of our study was to estimate the prevalence of overweight and obesity in the adolescent population of Barcelona and to analyse their association with inadequate eating habits and sedentary behaviours.
Materials and methodsStudy design and participantsA cross-sectional study was carried out using the FRESC self-reported questionnaire on health-related risk factors in secondary school students.18 In 2008 the questionnaire was administered to a representative sample of students of the second year of Educación Secundaria Obligatoria (compulsory secondary education [ESO]) (ages 13–14 years), the fourth year of ESO (ages 15–16 years), and the second year of de Bachillerato (post-compulsory secondary education) and of Ciclos Formativos de Grado Medio (middle-grade vocational training cycles [CFGM]) (ages 17–18 years) enrolled in public, private, and subsidised schools in Barcelona. The FRESC-2008 questionnaire includes questions about sociodemographic characteristics, substance use, interpersonal relationships, leisure, diet, sexuality and road safety. The questions were formulated based on previous versions of the same questionnaire and on other Spanish and international surveys, such as the Health Behaviour in School-Aged Children (HBSC) survey. Also, in 2008 objective weight and height measurements were obtained for the first time.18
We performed cluster randomised sampling, stratifying by the type of school (public or private/subsidised) and the socioeconomic status (SES) of the neighbourhood where schools were located (high, middle or low; based on the 1996 Indice de Capacidad Económica Familiar, or family income index [ICEF]).19 The sampling unit was the classroom. We estimated the sample size at 1250 by academic year for a sampling fraction of 10% of the population under study and assuming a 20% non-response rate. The survey was administered to the students of a total of 136 classrooms (49 of 2nd year of ESO, 49 of 4th year of ESO, and 38 of the 2nd year of Bachillerato-CFGM) in 80 secondary education schools in Barcelona.18
The questionnaire was administered between February and May of 2008 during regular school hours by specially trained personnel from the Agència de Salut Pública de Barcelona (Public Health Agency of Barcelona [ASPB]). The same staff measured the weight and height of the students when they had completed the questionnaire. The collected data were entered in the database using the application Teleform v10.2.
Study variablesThe dependent variable was the BMI (kg/m2), calculated from the weight and height of each student. Then, the BMI variable was coded into 4 categories: underweight, normal weight, overweight, and obesity based on the age-and-sex-specific cutoffs established by Cole et al.17,20
The sociodemographic variables we analysed were sex, age, individual SES and immigration history of the family. The individual SES of each student was assessed by means of the Family Affluence Scale (FAS) (as low, middle or high), an indicator of household wealth.21 The family immigration history was defined into three categories according to the birth place of the students and their parents: native (student, father and mother born in Spain), first generation immigrant (student born outside Spain), and second generation immigrant (student born in Spain to a mother and/or father born outside Spain). The variables concerning the school included in the analysis were the type of institution (public or private/subsidised) and the SES of the school (high, middle or low).19
The variables regarding diet were the breakfast pattern, intake of unhealthy foods, and dieting. The “breakfast” variable was measured based on two questions about having breakfast before leaving home and at mid-morning, and defined into four categories: always having breakfast before leaving the house and at mid-morning, always having breakfast either before leaving the house or at mid-morning, having breakfast sometimes but not daily before leaving the house or at mid-morning, and never having breakfast. The variable “intake of unhealthy foods” was defined as consuming sweets, sugary drinks or snacks 4 or more times per week (yes/no), based on the food pyramid guidelines.22 The variable “currently on a weight-loss diet” was defined as a dichotomous variable (yes/no).
The variables used to analyse sedentary behaviour and physical activity were regular (nearly daily) physical activity (yes/no) and total daily screen time (television, game console or computer). The latter was categorised into less than 2h a day, and 2 or more hours a day, as recommended by the American Academy of Pediatrics (AAP)23 and the Asociación Española de Pediatría (Spanish Association of Pediatrics [AEP]).
Statistical analysisWe calculated percentages for categorical variables and the mean and standard deviation for age. We compared percentages and means using the chi square test and the Mann–Whitney U test, respectively. Later on, we conducted bivariate and multivariate logistic regression analyses to identify the factors associated with overweight and obesity. We performed separate analyses for the two categories, and used the normal weight and underweight group as a reference. The multivariate analyses were adjusted for the variables that had shown a significant association and by age, FAS, type of school and SES of the school. In the multivariate logistic regression analyses we calculated the adjusted odds ratios (aOR) and their respective confidence intervals (95% CI). All the analyses were stratified by sex. All statistical analysis were conducted using STATA v10.
ResultsWe analysed the data of 3089 individuals (response rate, 87.2%), 52% of which were female, with a mean age of 15.8 years. Most of the students were natives (79.3%) and approximately 90% was of a middle or high SES. Of all students, 72.1% attended a private or subsidised school, and more than 80% attended a school in a middle or high SES neighbourhood (Table 1).
Sociodemographic characteristics of the sample, by sex. FRESCa 2008, Barcelona.
| Variables | Males | Females | P-valueb | Total |
|---|---|---|---|---|
| Mean (SD) | Mean (SD) | Mean (SD) | ||
| Age | 15.7 (1.69) | 15.8 (1.77) | .121 | 15.8 (1.74) |
| n (%) | n (%) | P-valuec | n (%) | |
| Family Affluence Scale (FAS) | ||||
| Low | 165 (11.3) | 196 (12.2) | .687 | 361 (11.8) |
| Middle | 640 (43.7) | 693 (43.4) | 1333 (43.5) | |
| High | 660 (45.0) | 709 (44.4) | 1369 (44.7) | |
| Family immigration historyd | ||||
| Native | 1176 (80.7) | 1234 (78.0) | .163 | 2410 (79.3) |
| 1st generation immigrant | 101 (6.9) | 130 (8.2) | 231 (7.6) | |
| 2nd generation immigrant | 180 (12.4) | 219 (13.8) | 399 (13.1) | |
| Type of school | ||||
| Private/subsidised | 1082 (72.9) | 1144 (71.3) | .312 | 2226 (72.1) |
| Public | 402 (27.1) | 461 (28.7) | 863 (27.9) | |
| School socioeconomic statuse | ||||
| High | 550 (37.1) | 219 (42.2) | .013 | 1227 (39.7) |
| Middle | 671 (45.2) | 130 (42.1) | 1347 (43.6) | |
| Low | 263 (17.7) | 252 (15.7) | 515 (16.7) | |
| Total (n) | 1484 | 1605 | 3089 | |
Native: student born in Spain to a mother and father born in Spain; 1st generation immigrant: student born outside Spain; 2nd generation immigrant: student born in Spain to a mother and/or father born outside Spain.
Socioeconomic status of the neighbourhood in which the school is located based on the Índice de Capacidad Económica Familiar (family income index [ICEF]).19
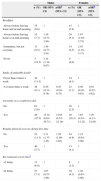
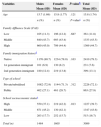
The prevalence of overweight and obesity was higher in male than in female students (19.9% for overweight and 6.2% for obesity in males, versus 17% for overweight and 3.7% for obesity in females; P<.001). When it came to breakfast, 19.1% of female students reported never having breakfast or having it only a few times a week, a higher percentage than the one observed in males (15.5%; P=.001). The proportion of students that reported being on a weight-loss diet was higher in females (18.4%) than in males (7.4%) (P<.001). Meanwhile, 66.5% of male students and 56.1% of female students reported consuming unhealthy foods in excess of the recommended occasional intake (P<.001). The proportion of male students that reported exercising regularly (60.2%) was much higher than the proportion of female students (28.9%) (P<.001). Approximately 80% of the youth reported 2 or more hours of screen time a day (Table 2).
Body mass index (BMI) and main associated variables (diet, sedentary behaviour and physical activity), by sex. FRESCa 2008, Barcelona.
| Variables | Males | Females | P-valueb | Total |
|---|---|---|---|---|
| n (%) | n (%) | n (%) | ||
| Body mass index (BMI)c | ||||
| Underweight | 12 (0.8) | 15 (0.9) | <.001 | 27 (0.9) |
| Normal weight | 1078 (73.1) | 1.250 (78.4) | 2328 (75.8) | |
| Overweight | 294 (19.9) | 271 (17.0) | 565 (18.4) | |
| Obesity | 92 (6.2) | 59 (3.7) | 151 (4.9) | |
| Breakfast | ||||
| Always before leaving home and at mid-morning | 646 (44.6) | 632 (39.9) | .001 | 1278 (42.1) |
| Always before leaving home or at mid-morning | 577 (39.9) | 650 (41.0) | 1227 (40.5) | |
| Sometimes, but not everyday | 190 (13.1) | 278 (17.5) | 468 (15.4) | |
| Never | 35 (2.4) | 25 (1.6) | 60 (2.0) | |
| Intake of unhealthy foodsd | ||||
| Fewer than 4 times a week | 485 (33.5) | 695 (43.9) | <.001 | 1180 (39.0) |
| 4 or more times a week | 961 (66.5) | 887 (56.1) | 1848 (61.0) | |
| Currently on a weight-loss diet | ||||
| Yes | 106 (7.4) | 291 (18.4) | <.001 | 397 (13.1) |
| No | 1335 (92.6) | 1293 (81.6) | 2628 (86.9) | |
| Regular physical exercise during free time | ||||
| Yes | 880 (60.2) | 460 (28.9) | <.001 | 1340 (43.8) |
| No | 583 (39.8) | 1.133 (71.1) | 1716 (56.2) | |
| Recreational screen timee | ||||
| <2h/day | 240 (19.7) | 301 (21.6) | .224 | 541 (20.7) |
| ≥2h/day | 978 (80.3) | 1090 (78.4) | 2068 (79.3) | |
Unhealthy foods: based on the consumption of sweets and chocolates, pasta, snacks and sugary drinks; categories based on the reference food pyramid for healthy nutrition designed by the Agència de Salut Pública de Barcelona (ASPB).22
Daily screen time: based on the dichotomous definition of the American Academy of Pediatrics (AAP) for time spent in front of a screen: 2h or more per day and less than 2h a day.23
Tables 3 and 4 present the results of the logistic regression analyses for overweight and obesity, respectively. Overweight was associated with the breakfast pattern in both sexes, increasing as breakfast decreased (having breakfast daily only once [males: aOR=1.39; 95% CI, 1.03–1.89; females: aOR=1.45; 95% CI: 1.05–2.01]; having breakfast only a few days a week [males: aOR=2.05; 95% CI, 1.35–3.12; females: aOR=1.65; 95% CI, 1.09–2.49]; and never having breakfast [females: aOR=4.07; 95% CI, 1.59–10.44]). A lower intake of unhealthy foods (males: aOR=0.63; 95% CI, 0.47–0.83; females: aOR=0.67; 95% CI, 0.50–0.89) and being on a diet (males: aOR=5.07; 95% CI, 3.07–8.38; females: aOR=4.59; 95% CI, 3.35–6.29) were also associated with overweight (Table 3).
Association between overweight (comparison group: normal weight or underweight) and eating habits and sedentary behaviours, by sex. FRESCa 2008, Barcelona.
| Males | Females | |||||
|---|---|---|---|---|---|---|
| n (%) | OR (95% CI) | aORb (95% CI) | n (%) | OR (95% CI) | aORb (95% CI) | |
| Breakfast | ||||||
| Always before leaving home and at mid-morning | 108 (17.8) | 1 | 84 (13.7) | 1 | ||
| Always before leaving home or at mid-morning | 122 (22.6) | 1.35 (1.01–1.80) | 1.39 (1.03–1.89) | 116 (18.7) | 1.46 (1.07–1.98) | 1.45 (1.05–2.01) |
| Sometimes, but not everyday | 51 (29.1) | 1.90 (1.29–2.80) | 2.05 (1.35–3.12) | 58 (22.3) | 1.82 (1.25–2.63) | 1.65 (1.09–2.49) |
| Never | 8 (26.7) | 1.68 (0.73–3.87) | 2.07 (0.86–4.98) | 9 (37.5) | 3.79 (1.61–8.94) | 4.07 (1.59–10.44) |
| Intake of unhealthy foodsc | ||||||
| Fewer than 4 times a week | 118 (26.8) | 1 | 136 (20.7) | 1 | ||
| 4 or more times a week | 173 (19.1) | 0.64 (0.49–0.84) | 0.63 (0.47–0.83) | 131 (15.3) | 0.69 (0.53–0.90) | 0.67 (0.50–0.89) |
| Currently on a weight-loss diet | ||||||
| No | 249 (19.6) | 1 | 159 (12.6) | 1 | ||
| Yes | 42 (56.8) | 5.39 (3.33–8.71) | 5.07 (3.07–8.38) | 108 (42.0) | 5.02 (3.72–6.76) | 4.59 (3.35–6.29) |
| Regular physical exercise during free time | ||||||
| No | 118 (22.4) | 1.12 (0.86–1.45) | 178 (16.5) | 0.78 (0.59–1.04) | ||
| Yes | 172 (20.6) | 1 | 89 (20.1) | 1 | ||
| Recreational screen timed | ||||||
| <2h/day | 49 (21.7) | 1 | 52 (17.8) | 1 | ||
| ≥2h/day | 189 (20.6) | 0.94 (0.66–1.34) | 180 (17.3) | 0.97 (0.69–1.36) | ||
Model adjusted for statistically significant variables and age, Family Affluence Scale, type of school and socioeconomic status of the school neighbourhood (based on the Índice de Capacidad Económica Familiar).
Unhealthy foods: based on the consumption of sweets and chocolates, pasta, snacks and sugary drinks; categories based on the reference food pyramid for healthy nutrition designed by the Agència de Salut Pública de Barcelona (ASPB).22
Daily screen time: based on the dichotomous definition of the American Academy of Pediatrics (AAP) for time spent in front of a screen: 2h or more per day and less than 2h a day.23
Association between obesity (comparison group: normal weight or underweight) and eating habits and sedentary behaviours, by sex. FRESCa 2008, Barcelona.
| Males | Females | |||||
|---|---|---|---|---|---|---|
| n (%) | OR (95% CI) | aORb (95% CI) | n (%) | OR (95% CI) | aORb (95% CI) | |
| Breakfast | ||||||
| Always before leaving home and at mid-morning | 35 (6.6) | 1 | 15 (2.8) | 1 | ||
| Always before leaving home or at mid-morning | 35 (7.7) | 1.19 (0.73–1.94) | 28 (5.3) | 1.97 (1.04–3.73) | ||
| Sometimes, but not everyday | 13 (9.5) | 1.49 (0.77–2.91) | 14 (6.5) | 2.45 (1.16–5.17) | ||
| Never | 5 (18.5) | 3.24 (1.16–9.07) | 0 (0.0) | – | ||
| Intake of unhealthy foodsc | ||||||
| Fewer than 4 times a week | 42 (11.5) | 1 | 34 (6.1) | 1 | ||
| 4 or more times a week | 48 (6.1) | 0.50 (0.33–0.78) | 0.45 (0.28–0.73) | 23 (3.1) | 0.48 (0.28–0.83) | 0.45 (0.25–0.82) |
| Currently on a weight-loss diet | ||||||
| No | 61 (5.6) | 1 | 28 (2.5) | 1 | ||
| Yes | 29 (47.5) | 15.18 (8.63–26.71) | 12.05 (6.55–22.18) | 29 (16.3) | 7.65 (4.43–13.22) | 7.29 (4.13–12.85) |
| Regular physical exercise during free time | ||||||
| No | 52 (11.3) | 2.11 (1.37–3.25) | 1.76 (1.08–2.85) | 44 (4.6) | 1.15 (0.63–2.08) | |
| Yes | 40 (5.7) | 1 | 15 (4.1) | 1 | ||
| Recreational screen timed | ||||||
| <2h/day | 13 (6.8) | 1 | 8 (3.2) | 1 | ||
| ≥2h/day | 57 (7.3) | 1.07 (0.57–1.99) | 39 (4.3) | 1.36 (0.63–2.96) | ||
Model adjusted for statistically significant variables and age, Family Affluence Scale, type of school and socioeconomic status of the school neighbourhood (based on the Índice de Capacidad Económica Familiar).
Unhealthy foods: based on the consumption of sweets and chocolates, pasta, snacks and sugary drinks; categories based on the reference food pyramid for healthy nutrition designed by the Agència de Salut Pública de Barcelona (ASPB).22
Daily screen time: based on the dichotomous definition of the American Academy of Pediatrics (AAP) for time spent in front of a screen: 2h or more per day and less than 2h a day.23
As shown in Table 4, obesity was also associated with a lower intake of unhealthy foods (males: aOR=0.45; 95% CI, 0.28–0.73); females: aOR=0.45; 95% CI, 0.25–0.82) and with being on a diet (males: aOR=12.05; 95% CI, 6.55–22.18; females: aOR=7.29; 95% CI, 4.13–12.85) in both sexes. In male students, there was also a positive association between not exercising regularly and being obese (aOR=1.76; 95% CI: 1.08–2.85) (Table 4).
DiscussionThe results showed a high prevalence of overweight (18.4%) and obesity (4.9%) in adolescents 13–18 years of age, with higher proportions found in males. Being overweight or being obese were associated with currently being on a weight-loss diet and a lower intake of unhealthy foods in both sexes. Furthermore, overweight adolescents reported not having breakfast every day more frequently than adolescents with normal or underweight.
The prevalence of overweight and obesity in our study is consistent with the prevalences found in other studies conducted in Spain that used the same cutoff points. The AVENA study found a prevalence of overweight of 20% in boys and 16% in girls 13–18 years of age in the 2001–2002 period. The prevalence of obesity was 5.7 and 3.8%, respectively.4 Similarly, a more recent study found a 16.4% prevalence of overweight and a 6.7% prevalence of obesity in adolescents 14–17 years of age.24 All these data confirm that excess weight in adolescents continues to be a public health problem in our context.
Several authors favour the hypothesis that breakfast is the most important meal of the day, as it enables adequate physical and psychological performance.25 Furthermore, skipping breakfast leads to energy intakes between meals that are not recommended, or to a greater calorie intake in the remaining meals of the day that may upset the energy balance and result in weight gain.10 Previous studies (Enkid8 and OBICE11) have identified light breakfast and not having breakfast regularly as risk factors for obesity in children and adolescents. In addition, other studies express the need to have a balanced breakfast containing dairy, carbohydrates, fruit and protein to prevent overweight and obesity.9 Likewise, our results show an association between not having breakfast daily and overweight, with an increasing trend in overweight in both sexes as the frequency of breakfast lowered. Thus, adolescents that reported always skipping breakfast were most likely to be overweight. While the association between obesity and skipping breakfast every day was not statistically significant, we observed the same direction in this association as with overweight. The lack of statistical significance may be due to low statistical power, as the sample of students with obesity was small.
When it comes to the intake of unhealthy foods, some authors suggest that intakes above the recommended frequency (less than once a week) are associated with weight gain.26,27 The cross-sectional design of our study does not allow us to establish the direction of the observed association, seemingly contradictory, between excess weight and a lower intake of unhealthy foods. It is possible that the lesser consumption of these foods is due to the students’ awareness of their excess weight, and not the other way around. This explanation is supported by the positive association also found in our study between being on a weight-loss diet and excess weight, especially in obese adolescents. It is likely that students with excess weight are aware of their weight being too high and try to compensate for and/or reduce their excess weight with different strategies, such as eating fewer unhealthy foods and being on some type of diet.
When it comes to screen time, the results of previous studies diverge. Some authors have described a positive correlation between screen time and BMI, while others suggest that there is no association or that the association is weak and is not clinically relevant.28 Our results did not show an association between overweight or obesity and longer-than-recommended screen times. As for physical activity, previous studies have demonstrated an association between overweight and obesity and low levels of physical activity.11,26 Consistent with this, our study found that obese male students exercised less frequently than their normal weight or underweight counterparts. However, we did not find this association in obese or overweight female students.
One of the main limitations of this study is that it is based on a self-reported questionnaire on risk behaviours, which may carry an information bias. However, the anonymity of the questionnaires contributes to minimising this type of bias, as it encourages a greater degree of honesty in answering questions.29 Another limitation is that its cross-sectional design does not allow us to establish causality in the observed associations. We found associations with variables that may cause weight gain (such as inadequate breakfast) and with variables that may be the consequence of weight gain (such as dieting or lower intakes of unhealthy foods). These associations should be further studied in longitudinal studies to assess the directionality of the association. Last of all, the lack of a consensus on the definition of overweight and obesity in adolescents poses barriers to the comparison of our results with those of previous studies. To minimise this limitation, we applied the criteria of Cole et al.,17,20 as they are based on several populations from different countries and they are widely used in the literature. These limitations notwithstanding, the study was conducted on a large and representative sample of the adolescent population of Barcelona. Furthermore, objective measurements of weight and height were taken, which guaranteed the validity of the dependent variable values (BMI).
The results of our study show that overweight and obesity continue to be a relevant public health problem in our environment, and reinforce the importance of having breakfast regularly to prevent or reduce excess weight. These results evidence the need to review and update existing health promotion programs, emphasising the importance of daily healthy breakfasts during adolescence, as this is a key period for the development and maintenance of healthy habits that will have a considerable influence in future adult health.
FundingThis study has been funded by l’Agència de Gestió d’Ajuts Universitaris i de Recerca of the government of the autonomous community of Catalonia (AGAUR SGR 2009-1345).
AuthorshipDr Manel Nebot passed away on October 18, 2012. This study would not have been possible without his effort, dedication and perseverance.
Conflicts of interestThe authors have no conflicts of interest to declare.
We are grateful for the invaluable collaboration of the participating centres, teaching staff and students in this study. We also want to thank the community health teams of every district, and Ester Teixidó and Laia Clemente for their help in fieldwork and data collection. This article is part of the doctoral dissertation of Xavier Garcia-Continente, carried out at the Universitat Pompeu Fabra (UPF) of Barcelona.
Please cite this article as: Garcia-Continente X, Allué N, Pérez-Giménez A, Ariza C, Sánchez-Martínez F, López MJ, et al. Hábitos alimentarios, conductas sedentarias y sobrepeso y obesidad en adolescentes de Barcelona. An Pediatr (Barc). 2015;83:3–10.