Cellulitis-adenitis syndrome is a well-known presentation of Group B Streptococcus (GBS) late-onset sepsis in children. Although face and neck are most frequently involved, other locations can also be affected. Inguinal presentation is uncommon, but it may be the first clinical manifestation of a GBS bacteremia. We present two cases of cellulitis-adenitis syndrome with inguinal involvement in two female infants with GBS late onset sepsis.
Case 1A 12-week-old female was born by Cesarean delivery at 34 gestational weeks due to intrauterine growth restriction (1100g at birth). GBS screening was not performed. On the seventh day of life, the neonate presented a respiratory distress syndrome and was diagnosed of an S. epidermidis bacteremia, receiving intravenous vancomycin for 7 days. She was discharged from hospital at 6 weeks of age. At 12 weeks old, the girl was readmitted with an erythematous, warm and indurated skin lesion in the right inguinal region, five hours of fever (38.5°C) and poor feeding. Laboratory tests showed 14,400WBC/mm with 71% of segmented neutrophils and C-Reactive Protein (CRP) of 2.2mg/dl. A right inguinal ultrasonography was carried out, revealing inflammatory changes in subcutaneous tissue and local adenopathies. Blood cultures were withdrawn, and the girl was started on cefotaxime. After 24h, GBS was isolated in blood cultures, and treatment was switched to ampicillin and gentamicin. CSF culture resulted sterile. Gentamicin was discontinued after 5 days, and ampicillin was administered for a total of 13 days. The inguinal swelling and fever resolved within 48h after initiating antibiotics.
Case 2A 13-week-old female was born prematurely at 34 gestational weeks due to premature rupture of membranes. GBS maternal status was unknown. A dose of corticosteroids was administered to the mother antepartum, followed by a dose of ampicillin to the girl after delivery. In the 13th week of life, the girl presented to hospital with fever, fussiness and a swelling erythematous region in the left inguinal skin, accompanied by local lymphadenopathy. Inguinal ultrasound confirmed soft tissue edema with inguinal adenopathy. Laboratory tests showed 25,300WBC/mm with 67% of segmented neutrophils, and CRP of 0.14mg/dl. Ampicillin and cefotaxime were started, and GBS was isolated from blood cultures. CSF culture resulted negative. After the isolation of GBS, cefotaxime was stopped and ampicillin was given for a total course of 14 days. Skin lesions resolved completely after 6 days of treatment.
Cellulitis-adenitis syndrome is a well-described presentation of GBS late onset sepsis that occurs in 2%–4% of cases. It has been considered as an early indicator of GBS bacteremia in infants of which 24%–33% present meningeal involvement.1,2 The age of onset ranges from 1 to 13 weeks.2,3 Most cases affect the face and neck regions, being inguinal involvement an uncommon presentation. To this day, only 9 cases of inguinal cellulitis-adenitis have been published in the literature (Table 1).1–10
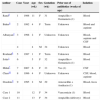
Clinical features, gestational age, prior use of antibiotics and source of isolation in children with inguinal GBS cellulitis-adenitis.
| Author | Case | Year | Age (wk) | Sex | Gestation (wk) | Prior use of antibiotics (weeks of age) | Isolation |
|---|---|---|---|---|---|---|---|
| Rand5 | 1 | 1988 | 11 | F | 31 | Ampicillin+Gentamicin (1) | Blood |
| Baker9 | 2 | 1982 | 4 | F | Term | Unknown | Blood and aspirate |
| Albanyan2 | 3 | 1998 | 2 | F | Unknown | Unknown | Blood, aspirate and CSF |
| 4 | 4 | M | 34 | Unknown | Blood | ||
| Rouland6 | 5 | 1987 | 1 | F | Term | Unknown | Blood |
| Soler1 | 6 | 5 | F | 32 | Ampicillin+Gentamicin (1) | Blood | |
| Mittal7 | 7 | 2007 | 6 | F | 33 | Yes (1) | CSF |
| Chen10 | 8 | 1996 | 4 | F | Unknown | Unknown | CSF, blood, aspirate |
| Doedens8 | 9 | 1995 | 2 | M | 29 | Amoxicillin+Amikacin (1) | Blood, feces |
| Case 1 | 10 | 12 | F | 34 | Vancomicin (1) | Blood | |
| Case 2 | 11 | 13 | F | 34 | Ampicillin (delivery) | Blood | |
Besides the cutaneous lesion, clinical presentation does not differ from other GBS infections, with fever, poor feeding, and fussiness. As described in the cervical region, the rate of meningeal involvement in inguinal cellulitis-adenitis is high (27%) (Table 1), therefore a lumbar puncture is mandatory in order to rule out meningitis. A previous history of preterm delivery and/or perinatal antibiotic treatment is present in most inguinal cases, being also associated with other manifestations of late-onset GBS disease.4,9 Particularly striking is the predominance of the female gender in inguinal cellulitis-adenitis syndrome (9/2). The pathogenesis of this finding may be related to an early colonization of female vaginal mucosa, leading to an initial inflammatory response in the lymph nodes, followed by bloodstream dissemination. This hypothesis could also be an explanation for the delay between the onset of local symptoms (cellulitis-adenitis) and clinical manifestations of sepsis.
In conclusion, inguinal cellulitis-adenitis is a poorly-understood manifestation of a GBS late-onset sepsis, taking place in children under 4 months of age. In most cases it presents as a bacteremic disease with high rates of meningeal involvement. Thus, having a high index of suspicion is of paramount importance for an early recognition of the disease and to establish appropriate antibiotic therapy.
Our thanks are due to Mr. Martin J. Smyth, B.A., for his help in correcting the English.
Please cite this article as: Blázquez D, Santiago B, Ruiz-Contreras J. An Pediatr (Barc). 2015;82:433–434.