The ingestion of magnetic objects can cause complications in children, and there are no epidemiological or clinical data on the subject in Spain.
ObjectivesTo determine the incidence, epidemiological characteristics and management of magnet ingestion in paediatric emergency departments in Spain.
Material and methodsProspective observational multicentre study conducted over a 3-year period. The study universe consisted of patients aged less than 14 years.
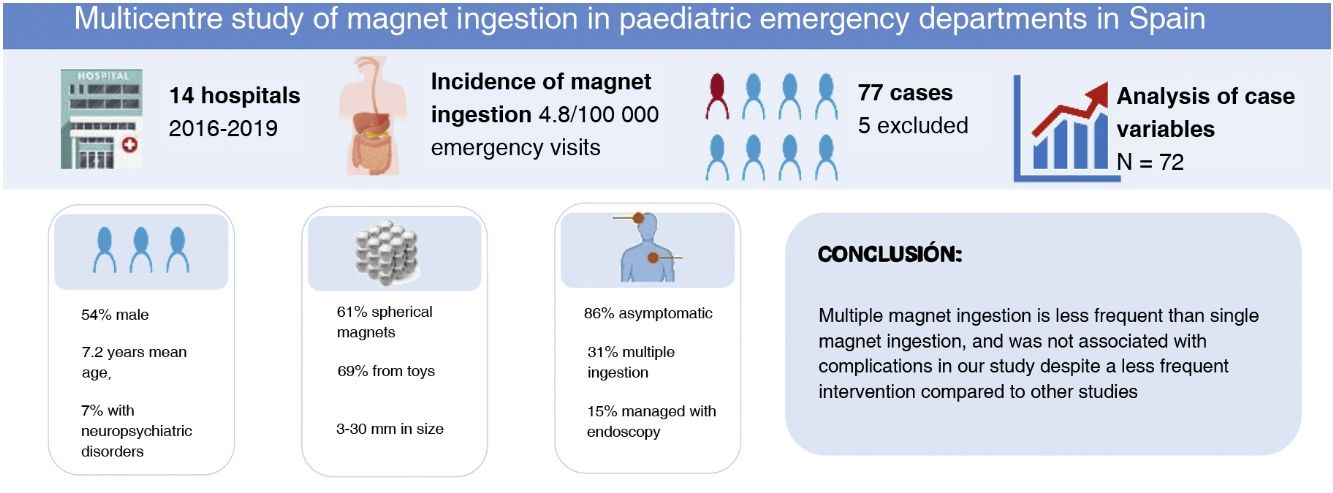
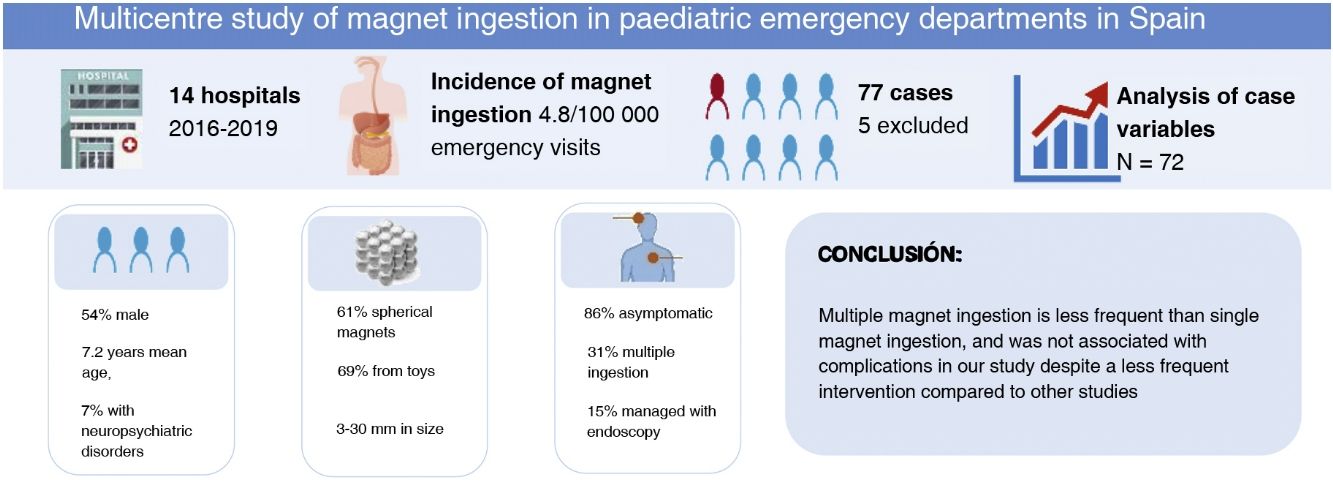
ResultsThe incidence was 4.8 cases per 100 000 emergency care episodes. Of the 72 patients included (mean age, 7.2 years), 54% were male. Seven percent had neuropsychiatric disorders. Sixty-one percent of the magnets were spherical and 69% came from toys. The size was variable, most frequently between 5 and 10 mm (50%), and ranging from 3 to 30 mm. Eighty-six percent of patients were asymptomatic. The most frequent symptom was abdominal pain. Eighty-three percent of the patients sought medical care within 6 h of ingestion and 92% within 24 h. Thirty-one percent of the cases were of multiple ingestion. Endoscopy was required for extraction in 15% of cases, a proportion that rose to 36% in the group of cases of multiple ingestion. None of the patients required surgery. We did not observe any gastrointestinal complications of magnet ingestion.
ConclusionsThe ingestion of multiple magnets is less frequent than single magnet ingestion, and we did not observe any complications despite the lower frequency of procedures compared to other studies.
Las ingestas de objetos imantados pueden presentar complicaciones en el niño, no existiendo datos epidemiológicos ni clínicos en España.
ObjetivosConocer la incidencia de ingesta de objetos imantados en los Servicios de Urgencias Pediátricos Españoles, sus características epidemiológicas y su manejo.
Material y métodosEstudio observacional prospectivo multicéntrico realizado durante 3 años. Población de referencia menores de 14 años.
ResultadosLa incidencia fue de 4,8/100.000 urgencias. De los 72 pacientes incluidos (edad media de 7,2 años), el 54% fueron varones. El 7% presentaron antecedentes neuropsiquiátricos. El 61% de los imanes fueron esféricos y el 69% procedían de juguetes. El tamaño fue variable con un predominio de los imanes entre 5 y 10 mm (50%). El 86% fueron asintomáticos. El síntoma más frecuente fue el dolor abdominal. El 83% de los pacientes consultaron en menos de 6 horas y el 92% en las primeras 24 horas. El 31% fueron ingestas múltiples. El 15% precisó intervención endoscópica, cifra que ascendió al 36% en los casos de ingestas múltiples. No se realizó ninguna intervención quirúrgica. No se observó ninguna complicación gastrointestinal secundaria.
ConclusionesLas ingestas de imanes múltiples son menos frecuentes que las simples y en este estudio no se han observado complicaciones a pesar de que las intervenciones realizadas han sido menores que en otros estudios.
The importance of suspecting and being aware of magnet ingestion rests on the potential complications of multiple ingestion. From an epidemiological standpoint, this has become a significant hazard from the mass-production and sales of rare earth magnets. Neodymium magnets are the strongest type of permanent magnets and produce significantly larger magnetic fields; they can be miniaturised and produced in different shapes (discs, blocks, rings, spheres and cubes), which has led to their ubiquitous use in items such as desk accessories,1 toys, or piercings and jewellery in general.2
Based on the recommendations of the North American Society for Pediatric Gastroenterology, Hepatology and Nutrition (NASPGHAN),3 in the case of multiple ingestion and location of the magnets (or a magnet and a metallic foreign body [FB]) in the oesophagus or stomach, the most appropriate management seems to be urgent endoscopic removal, even if the patient is asymptomatic. If FBs are distal to the stomach and the patient is asymptomatic, a possible alternative that can be contemplated is removal with colonoscopy or, if removal is not possible, watchful waiting with follow-up imaging. If there is no progression or the patient is symptomatic, surgical removal should be performed on an emergency basis.4 However, it is not always possible to determine whether one or more magnets have been ingested if the magnets have clumped together.5 A few published works advocate for algorithms based on close inpatient observation in the case of multiple ingestion if there is evidence that the magnets have clumped together on arrival to the emergency department and the patient is asymptomatic on account of the potential risk of complications more invasive management.6,7 Despite the potential repercussions we have just mentioned, we did not find any studies in the literature that focused specifically on the clinical and demographic characteristics of paediatric patients presenting with magnetic FB ingestion.
The aim of our study was to establish the incidence of magnet ingestion in the population served by paediatric emergency departments in Spain and analyse the epidemiological variables that can help elucidate the circumstances surrounding the event more precisely and the clinical variables that may be associated with outcomes and management.
Material and methodsWe conducted a multicentre retrospective observational study with the participation of 14 paediatric emergency departments members of the research network of the Sociedad Española de Urgencias de Pediatría (Spanish Society of Paediatric Emergency Medicine) (RiSEUP-SPERG). It was a longitudinal study that started in November 2016 (after the recruitment of participating centres) and ended in October 2019. The study universe were patients aged less than 14 years managed in participating emergency departments. The inclusion criteria were magnetic FB ingestion as reason for visiting the emergency department and written informed consent. The exclusion criteria were refusal to participation in the study or failure to complete the informed consent form. The study was approved by the Clinical Research Ethics Committee of the Basque Country (the competent committee for the principal investigator). Data were collected in a restricted access database in adherence to current legislation. Variable validation criteria were established in order to minimise errors in data collection.
We calculated the incidence of FB ingestion (international classification of diseases [ICD], Spanish version codes: ICD-9 code 938, ICD-10 code T189XXA8) and of magnetic FB ingestion by a descriptive analysis of the variables in the identified cases. To assess the presence of statistically significant associations between groups in the tabulated categorical variables, we used the chi square test or, if the expected cell count for any category was less than 5, the Fisher exact test. We assessed for differences between 2 groups in the mean of continuous variables with the Student t test. We considered P-values of less than .05 statistically significant.
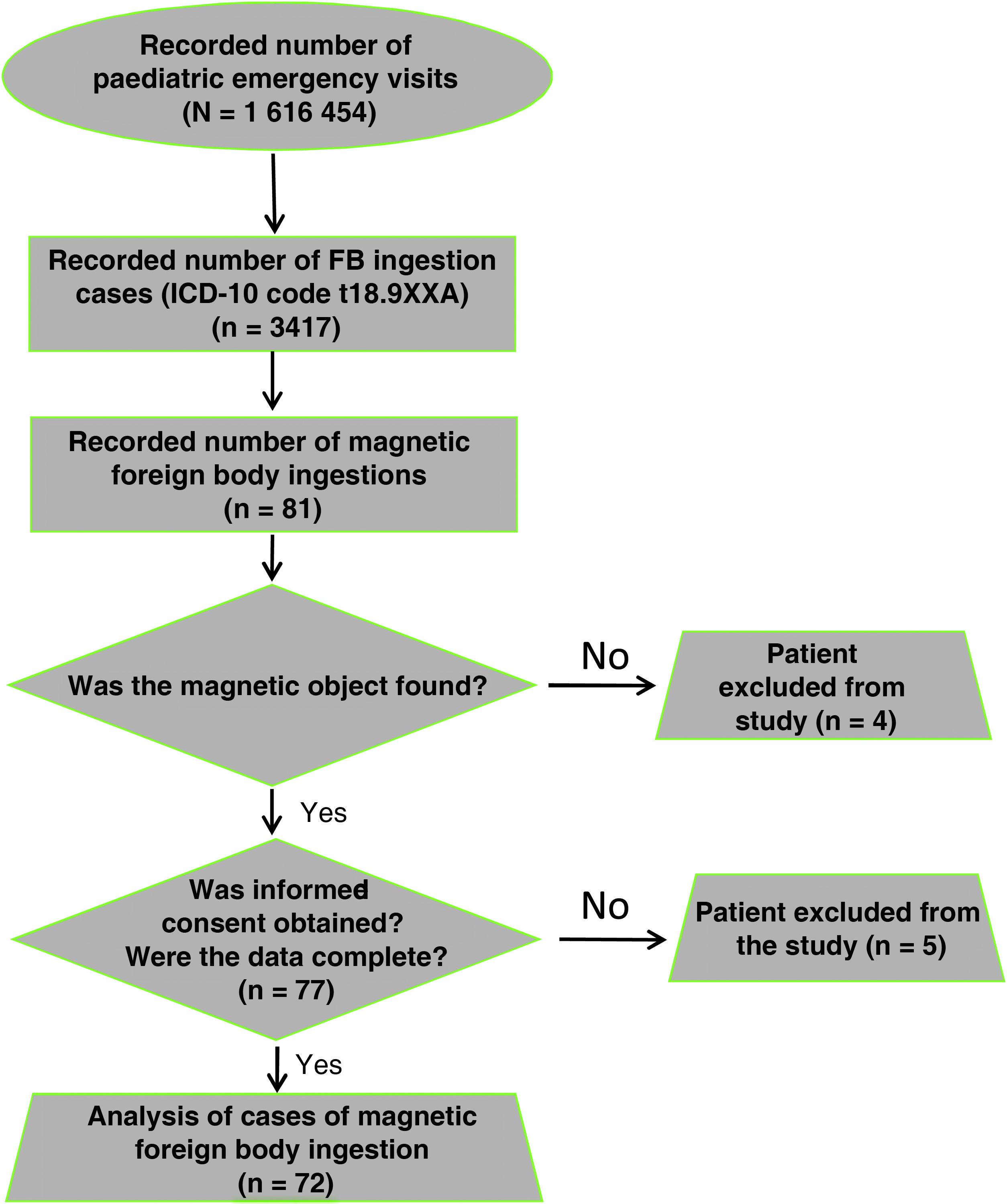
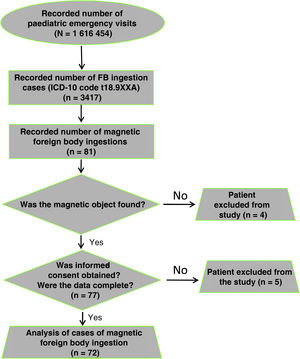
ResultsThe incidence of magnet ingestion in the population managed in Spanish paediatric emergency departments in the period under study was of 4.8 cases per 100 000 (4.7/100 000 in year 1 of the follow-up, 4.3/100 000 in year 2 and 5.3/100 000 in year 3). Cases of FB ingestion amounted to 0.21% of the total emergency care episodes. Magnetic objects were involved in 2.3% of the total cases of FB ingestion. Fig. 1 presents a flow chart of the study sample.
The descriptive analysis included 72 patients, as 5 cases were excluded (4 due to lack of informed consent and 1 due to failure to collect the minimum necessary data). The mean age was 7.2 years (standard deviation, 3.8 years) and the median 6.1 years (interquartile range, 4.7–10.4). Fifty-four percent (39) were male. In the subset with multiple ingestion (n = 22), the mean age was 8.6 years (standard deviation, 4.1 years) and the median age 9.8 years (interquartile range, 5.2–12.5); 45.5% (10) were male. We did not find a statistically significant difference in the incidence of multiple magnet ingestion based on sex (P = .325).
Five cases of magnet ingestion (7%) corresponded to patients with diagnosed neuropsychiatric disorders: 2 with neurodevelopmental delay, 2 with attention-deficit hyperactivity disorder and 1 with TDAH and 1 with giftedness and conduct disorder. We did not find significant differences in the frequency of multiple magnet ingestion (P = .638), the size of the ingested magnetic objects (P = .336) or the time elapsed until seeking care (P = .832) in the subset of patients with neuropsychiatric disorders.
Five percent of the cases (2) occurred in children with underlying gastrointestinal disorders: 1 with persistent constipation and 1 with an anorectal malformation (Table 1).
Clinical and demographic characteristics of patients with magnet ingestion (n = 72).
| Age | |
| <3 years | 8 (11%) |
| 3−6 years | 33 (46%) |
| >6 years | 31 (43%) |
| Source of magnets | |
| Toys | 50 (69%) |
| Jewellery | 4 (6%) |
| Kitchen | 4 (6%) |
| Other/not documented | 14 (19%) |
| Magnet size | |
| <5 mm | 8 (11%) |
| 5−10 mm | 36 (50%) |
| >10 mm | 22 (31%) |
| Not documented | 6 (8%) |
| Symptoms (not mutually exclusive) | 10 (14%) |
| Abdominal pain | 5 (7%) |
| Vomiting | 3 (4%) |
| Sore throat | 2 (3%) |
| Cough | 2 (3%) |
| Time to care-seeking | |
| <6 h | 60 (83%) |
| 6−24 h | 6 (8%) |
| >24 h | 4 (6%) |
| Not documented | 2 (3%) |
| Management | |
| Observation at home | 56 (78%) |
| Inpatient observation | 5 (7%) |
| Active intervention | 11 (15%) |
As regards the characteristics of the magnets, 61% (44) were spherical, and 69% (50) were from toys. They varied in size, with a predominance of magnets measuring 5–10 mm (50%), without statistically significant differences in management based on the size of the magnet (P = .498). The size of ingested magnets ranged from 3 to 30 mm.
In 49% of cases (35), there were witnesses to the ingestion. We did not find statistically significant differences in the frequency of witnesses between the cases of multiple and single magnet ingestion (P = .504).
All patients were deemed stable on arrival to the paediatric emergency department based on the paediatric assessment triangle. Eighty-six percent (62) were asymptomatic. The most frequent symptom was abdominal pain, and there were no statistically significant differences in the presence of symptoms based on magnet size (P = .098).
Eighty-three percent of patients (60) visited the emergency department within 6 h of ingestion, and 92% (66) within 24 h. The maximum time elapsed from ingestion to seeking emergency care was 13 days. When we assessed whether care seeking was delayed in the subset of patients with multiple magnet ingestion, we did not find statistically significant differences compared to single magnet ingestion (P = .795).
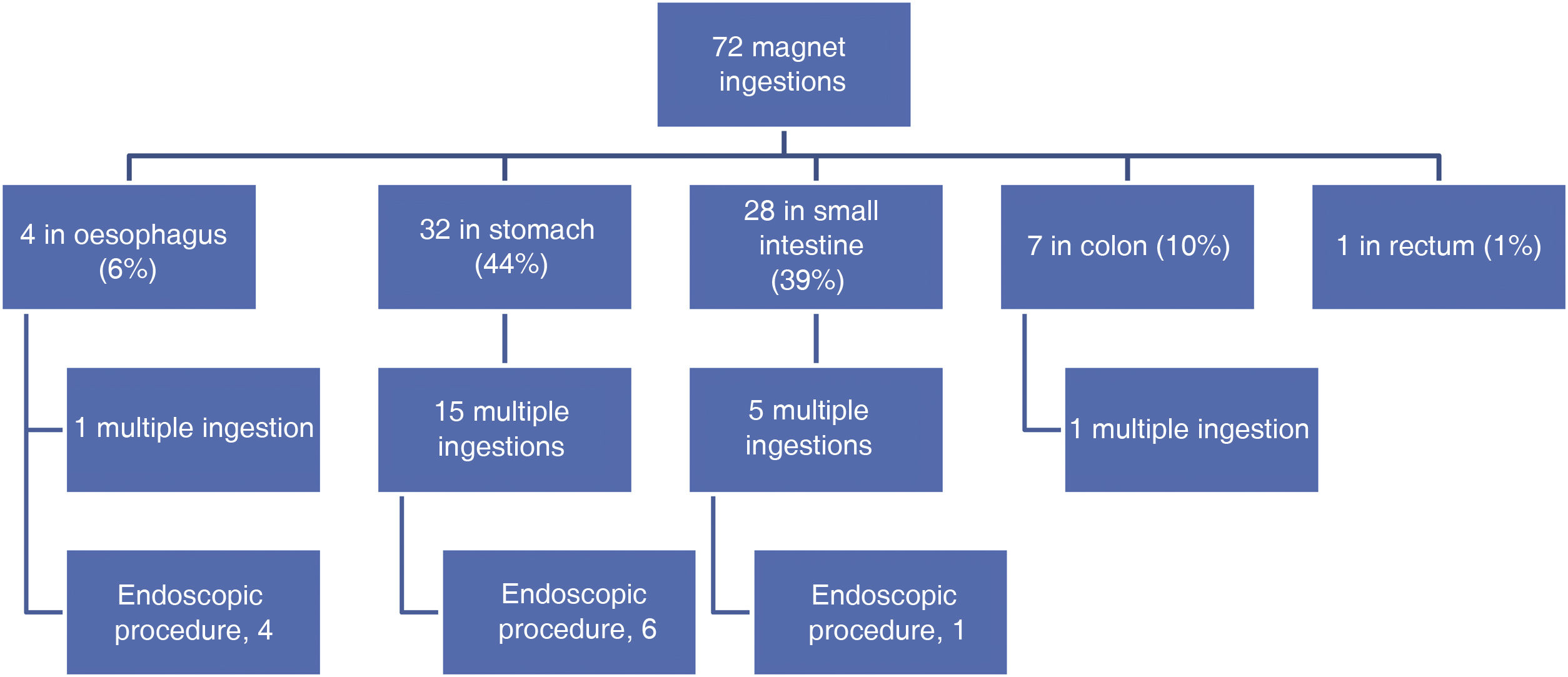
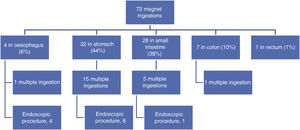
We found a statistically significant correlation between the time elapsed from ingestion to seeking emergency (categorised into less than or more than 6 h) and the location of the FBs on arrival to the emergency department (P < .001). In every case in which the magnetic objects could be removed endoscopically (located in oesophagus or stomach), the patients presented to the department within 6 h of ingestion. Fig. 2 presents the distribution of the location of the magnets on arrival to the emergency department.
Sixty-nine percent of the cases of magnet ingestion (50) involved a single magnet, and in this subset of cases, 6% (3) required removal due to the oesophageal location of the magnet, which did not result in any complications.
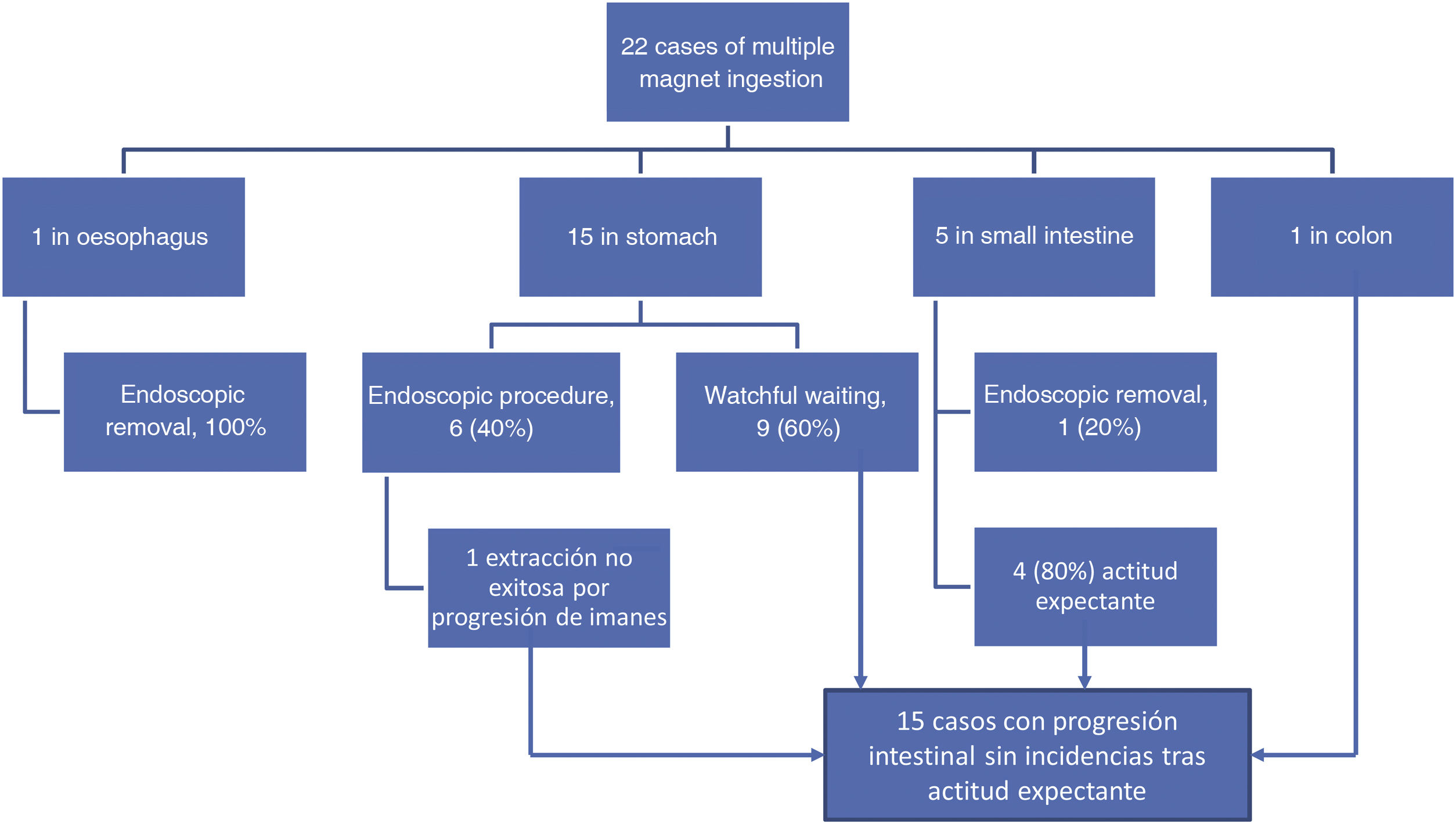
There were 22 cases of multiple magnet ingestion (31%). Thirteen corresponded to ingestion of 2 magnets and nine to ingestion of more than 2 magnets, with a maximum of 9 ingested magnets. In 82% of cases of multiple magnet ingestion (18), the magnets came from toys.
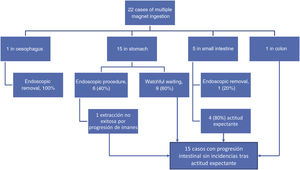
In the subset of multiple magnet ingestion, 8 cases (36%) were managed invasively, in every instance with endoscopy. Open surgery was not used in any case. All endoscopic procedures were successful, with the exception of one due to FB migration. All patients that underwent endoscopic intervention except one were asymptomatic. Nine cases of multiple magnet ingestion were managed with watchful waiting, as all appeared to be clumped together in the imaging tests performed on arrival to the department. Of these 9 cases, one third (3) involved ingestion of more than 2 magnetic FBs, and although they were not actively removed, they were eventually eliminated without complications. Fig. 3 presents the approach to the management and outcomes of multiple magnet ingestion cases.
The frequency of endoscopic removal was significantly higher in the group of multiple magnet ingestion cases compared to single magnet ingestion (P < .001). In the subset of multiple magnet ingestion, we did not find statistically significant differences between different groups despite differences in the accessibility of the magnets (P < .351).
None of the patients were found to have developed complications in the follow-up conducted by telephone 1 month after discharge from the paediatric emergency department.
DiscussionTo date, the incidence of magnetic FB ingestion in Spain had remained unknown, although there was concern due to the increase observed in recent years in other countries. Among the studies conducted in the United States, Abbas et al. reported an estimated increase in incidence from 0.45 cases per 100 000 emergency visits in 2002 to 3.75 per 100 000 emergency visits in 2011.9 Silverman et al. reported similar results,10 with 73% of magnet ingestion cases and 91 % of multiple ingestion cases occurring from 2007. Tavarez et al. estimated an incidence of 10 cases per 100 000 paediatric emergency visits between 2003 and 2009.11 Brown et al. reported that the incidence of magnet ingestion-related emergency visits reached 26 per 100 000 visits between 2010 and 2012.12 And in a series published by Waters et al., 71% of cases of magnet ingestion occurred after year 2010.13
In light of this increase in cases, and despite the use of warnings and structured changes in the packaging of magnetic toys, and given the persistence of the increase in related morbidity, certain desk accessories were recalled from the market and legislation established to mandate a sufficiently large size and restrictions to magnetic field strength to prevent complications following accidental ingestion.14 Later on, in 2016, following a court ruling against these mandates, more potent and smaller magnets entered the market. Reeves et al. assessed the impact of regulatory measures and concluded that following the implementation of bans, the incidence of magnet ingestion decreased,15 but subsequently started increasing again from 2016.16 A study by Middleberg et al. found an initial descent that was, however, followed by a 39% increase in 2018–2019 relative to 2008.17
In Canada, Strickland et al. described an incidence of 10 per 100 000 emergency visits in 2010 that increased to 34 per 100 000 in 2012.18 There was a clear improvement in these figures following the recall of some adult desk toys containing mini-magnets.19
In Asia, several recently published articles reflect concern regarding the incidence of magnet ingestion in the paediatric population. In Japan, Miyamoto et al. have estimated an incidence of 50–70 cases a year.20 A multicentre study conducted by Wang et al. in China in 2020 found that the number of cases increased by 9-fold in 2017 and 2018 compared to 2013 and 2014.21
As regards Europe, a multicentre retrospective study with a 5-year follow-up conducted by Talvard et al. in France (2015) included 40 cases of magnetic ingestion.22
In our study, the only multicentre study conducted in Spain in the current literature, the incidence was of 4.8 per 100 000 emergency visits during the follow-up period. The incidence did not vary significantly through the 3 years of data collection, but this is time window is short for the observation of changes in temporal trends. Data from long-term studies would be useful to reach this conclusion with greater certainty. In agreement with the previous literature, magnet ingestion was more frequent in boys11,18,20,22 and children under 6 years.9,13,18,20 Other articles have also reported an association between greater age and multiple ingestion,9,11,12 which was also the case in our study. In agreement with previous reports, most of the magnets came from toys.22 Seven percent of patients had neurodevelopmental disorders; in the previous literature, this proportion from 5%18 to 25%,12 and the number of cases in our study was too small to draw firm conclusions. The time elapsed from ingestion to seeking emergency care was shorter compared to other studies13,21 and was associated with the accessibility of magnets on arrival to the emergency department. The majority of patients in other studies were also asymptomatic, and the most frequent symptom was abdominal pain.12 As regards the type of magnet ingestion, in our study we found a predominance of single magnet ingestion, and this outcome varies between studies, as some found a predominance of single magnet ingestion10,11,20 and others of multiple magnet ingestion,12,22 with no apparent association with a given geographical location. Despite the publication of management guidelines by important scientific societies, such as the NAPGHAN,3 our study continued to find differences between providers in the management of these patients. One salient finding was the low proportion of endoscopic intervention in cases of multiple magnet ingestion with gastric location, in spite of which there were no subsequent gastrointestinal complications. However, it is important to consider that in every case the magnets appeared to be clumped together and the patients were asymptomatic on arrival to the emergency department, which could be related with the low incidence of complications observed. In our study, only 15% of magnet ingestion cases required endoscopic intervention, a proportion that rose to 36% in cases of multiple magnet ingestion, which was still below the proportion reported for multiple magnet ingestion in other studies, which ranges from 42% to 88%.11,12,20,22 We ought to underscore that every hospital should have a specific protocol for the management of magnet ingestion in the emergency department in coordination with the department of paediatric surgery. In addition to the importance of management, prevention plays a key role in this clinical condition. Measures should be designed to address consumption and educate the population to prevent and decrease the frequency of these events.
One of the possible limitations of the study is that the data may not be extrapolated to the entire population of Spain. The database only includes records of patients managed in emergency departments, therefore excluding visits to primary care centres and small medical facilities in the geographical areas covered in the study, which may have led to the underestimation of the actual incidence of magnet ingestion.
ConclusionThe incidence of magnetic foreign body ingestion in Spanish paediatric emergency departments during the period under study was of 4.8 cases per 100 000 emergency care episodes. Multiple magnet ingestion was less frequent than single magnet ingestion, and was not associated with complications in our study, even though they were managed less aggressively compared to other studies. A nationwide register of magnet ingestion cases may be needed to obtain more significant data of their potential complications by increasing the number of documented cases.
FundingThe study was funded through the 2016 annual grant of the Research Network of the Sociedad Española de Urgencias de Pediatría (RiSEUP-SPERG), for an amount of euro4000.
Conflicts of interestThe authors have no conflicts of interest to declare.