Introduction
The events surrounding the delivery process have a profound impact on morbidity and mortality of extremely premature infants 1. The incidence of severe intraventricular hemorrhage (IVH), periventricular leukomalacia (PVL) and mortality are all influenced by numerous prenatal and postnatal variables 2,3. Delivery room cardiopulmonary resuscitation (DR-CPR) is an event likely to influence these outcomes but has not been included as a risk factor in short and long-term outcome studies.
Current neonatal resuscitation guidelines consider appropriate the non-initiation of resuscitation for newborns of less than 23 weeks confirmed gestational age and/or less than 400 grams at birth 4,5. Above this threshold of viability, DR-CPR is routinely performed on critically ill premature infants despite controversial evidence of risk/benefit ratio for those who receive such therapy 6,7 and ethical dilemmas surrounding this practice 8,9.
Neonatal resuscitation in the premature infant can be divided in two distinct scenarios: resuscitation performed in the neonatal intensive care unit 10-12 and resuscitation performed in the delivery room during the first minutes of postnatal life 13,14. Each resuscitation experience has very distinct implications in mortality and morbidity among those who survive.
Long-term outcome data in very low birth weight (VLBW) infants exposed to DR-CPR are limited to two single center descriptive studies 13,14 that combined describe only a total of 16 infants.
We performed this study with the specific aim of determining if resuscitation in the delivery room in infants born with a birth weight ≤ 1,250 grams is a predictor of poor short-term outcomes (Severe IVH, PVL and death) and/or of poor long-term outcomes, as assessed by the Bayley Scales of Infant Development-II scores. Our hypothesis was that DR-CPR in infants born with birth weight ≤ 1,250 grams is a predictor of both poor short-term outcomes and poor neuromotor and cognitive outcomes at 18 months corrected age.
Methods
After obtaining approval from the Institutional Review Board at Emory University, we performed a retrospective cohort study of infants with birth weight ≤ 1,250 grams born at two perinatal centers in Atlanta, GA (Grady Memorial Hospital (GMH) and Emory Crawford Long Hospital) during a four year period (January 1st, 2000 to December 31st, 2003). Both hospitals were staffed by the same Emory University faculty and neonatal nurse practitioner group. The major difference between the centers was that at GMH there is full time resident coverage. However, a senior team member (senior Fellow, Neonatologist and/or NNP) is always in attendance at delivery for these high risk VLBW infants at both centers. This study period was chosen because we aimed to study a recent cohort were there were no major changes in general perinatal practices or in hospital specific protocols. In addition, our objective was to include infants who would be eligible for detailed follow up at 18 months post conceptional age. The data was obtained from our perinatal database and chart review performed for all infants who met inclusion criteria. We excluded infants with major congenital anomalies, outborn infants, and infants who were not offered resuscitation measures and received only "comfort care" until their demise.
The predictive variable was DR-CPR; infants were considered to have received DR-CPR if in addition to intubation and ventilation, chest compressions and/or epinephrine were given in the delivery room. Short-term outcome variables measured were death, severe IVH and PVL at any time before discharge from the neonatal intensive care unit. Combined poor short-term outcome was defined as the presence of death and / or severe IVH and/or PVL at any point during the hospital stay. Severe IVH was defined as grade III or IV intraventricular hemorrhage based on Papille's classification 15 on cranial ultrasound done at day of life 7 and read by pediatric radiologists who were unaware of DR-CPR exposure. PVL was diagnosed by screening cranial ultrasound performed at around one month of age that were consistent with cystic changes and or hyper-echogenic areas in the periventricular region. The results of the ultrasounds were prospectively collected on the database and only those infants that had ultrasound screening were included in the denominator for the analysis of severe IVH and PVL.
For long-term outcomes we included the infants ≤ 1,250 grams who survived to discharge during the same study period and were seen for neurodevelopmental follow-up at 18 months corrected age. Long-term outcome variables were assessed by the Bayley Scales of Infant Development-II scores 16-18 at 18 months corrected age. These measurements consisted of two scores, the Mental Developmental Index (MDI) and the Psychomotor Developmental Index (PDI). The mean and standard deviation for these scores are 100 ± 15 and infants are considered to be significantly delayed if the MDI or PDI score is ≤ 70, or an equivalent to two standard deviations below the mean 16-18.
Neonatal demographics included birth weight, gestational age, small for gestational age (birth weight less than the 10th percentile for gestational age), gender, race, and Apgar scores at 1 and 5 minutes of age. We also analyzed perinatal variables that included the use of antenatal steroids, multiple gestation, mode of delivery, breech presentation, prolonged rupture of membranes (rupture of membranes for more than 18 hours prior to delivery), chorioamnionitis (pathology report) and maternal administration of magnesium sulfate used for preterm labor and/or pregnancy induced hypertension. Gestational age was assigned by the best obstetrical estimate, based on the last menstrual period and/or early fetal ultrasound when available. If the best obstetrical estimate was not available or there was significant discrepancy between maternal dates and ultrasound results, we used the modified Ballard exam 19 as recorded in the admission note of the medical record to determine gestational age.
Discrete demographic data were summarized with proportions and frequencies and continuous data with means and standard deviations. Univariate analyses were performed with Chi square test for categorical variables, Fisher's exact test when expected cell counts were less than five. Student's t-test was used for continuous variables and to compare mean MDI and PDI scores between the two groups. Multivariable logistic regression models were used to obtain adjusted odds ratios (OR) with 95 % confidence intervals, comparing outcomes between those infants that received DR-CPR and those who did not. We planned a priori to analyze the relations between the predictive and outcome variables in the entire cohort (all infants ≤ 1,250 grams), in the surviving infants and also by birth weight specific categories of 250 grams each. Variables which were biologically relevant and/or statistically different between the two groups in the cohorts or in any 250 grams category, were included as covariates in the logistic regression model (i.e. birth weight, gender, mode of delivery, use of antenatal steroids and multiple gestation). Statistical significance was set at 0.05. Statistical analyses were performed using Statistical Analysis System software (Version 8.02; SAS Institute Inc, Cary, NC).
Results
Short term outcomes
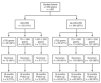
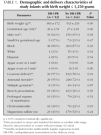
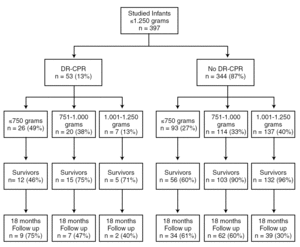
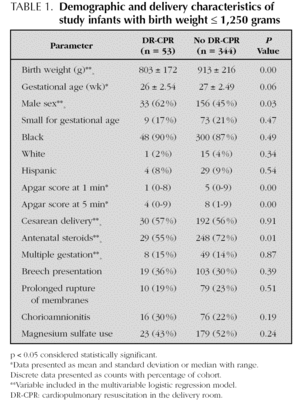
During the four year period, a total of 529 infants with a birth weight ≤ 1,250 grams were admitted to the two perinatal centers. We excluded 95 outborn infants, 32 infants who died after receiving only "comfort care measures", and 5 infants with a major congenital anomaly. Therefore, 397 infants met inclusion criteria for the short-term outcome analyses. Fifty three (13 %) infants received DR-CPR and 344 (87 %) did not. The description of the cohort and the distribution by 250 gram birth weight intervals is shown in figure 1. The number of cesarean deliveries, multiple gestations and mean gestational age were similar between the groups. Infants not receiving DR-CPR were more likely to be female and of higher birth weight and to have received antenatal steroids. As expected, infants not receiving DR-CPR had higher Apgar scores at 1 and 5 minutes of life (table 1).
Figure 1.Number of Infants Studied (DR-CPR and no DR-CPR).Total: 529 infants; outborn: 95 infants; comfort care only: 32 infants; major congenital anomalies: 5 infants.In each box: the sample size and percentage of infants are provided for each cohort or subcohort.RCP-SP: FALTA TRADUCIR LÍNEA.
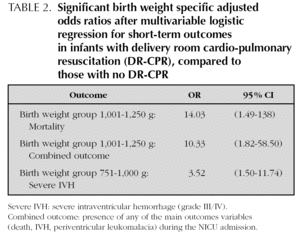
Among infants born between 1,001 to 1,250 grams, there were statistically significant differences in outcomes after multivariable regression analysis. Mortality was 29 % in the DR-CPR group compared to 4 % of those not requiring DR-CPR (OR 14.03, 95 % CI 1.49-138) and combined poor short-term outcome occurred in 43 % of infants receiving DR-CPR compared to 9 % (OR 10.33 95 % CI 1.82-58). In infants born between 751 to 1,000 grams, DR-CPR was associated with an increased risk of Severe IVH (OR 3.52, 95 % CI 1.50-11.74); 37 % of infants receiving DR-CPR developed severe IVH compared to 12 % of those not requiring DR-CPR (table 2).
Of the original cohort, 323 infants survived to discharge from the neonatal intensive care unit. Thirty two of them (10 %) had received DR-CPR and 291 did not. Among infants surviving to discharge, severe IVH was identified in 19 % of infants receiving DR-CPR compared to 7 % of infants who were not resuscitated. PVL occurred with the same frequency in both groups, about 3 %. A combined poor short-term outcome was seen in 21 % of the DR-CPR group compared to 9 % in the non-DR-CPR group. In the smallest infants (≤ 750 grams) there were only 12 survivors among those who received DR-CPR. Nine (75 %) of them had no evidence of severe IVH or PVL compared to 49 (88 %) of the 56 survivors requiring no resuscitation.
Long term outcomes
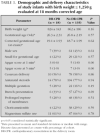
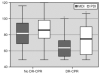
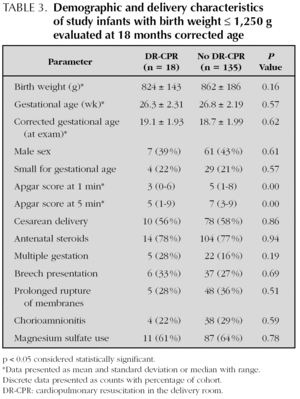
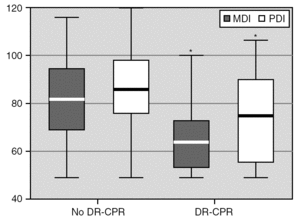
Long-term developmental evaluation was performed at 18 month post conceptional age in 18 (56 %) of the infants who had received DR-CPR and in 135 (42 %) who had not (fig. 1). Demographic data for these infants are shown in table 3. Other than Apgar scores, there were no statistically significant differences between the surviving infants in the DR-CPR and non-DR-CPR groups. Subjects lost to follow-up did not differ between the two study groups with regards to demographic variables or severity of illness. The mean Bayley Scales of Infant Development-II scores (fig. 2) were significantly worse in infants who survived after DR-CPR compared to non-DR-CPR survivors (67.7 ± 18.3 vs. 81.3 ± 17.7; p = 0.006). Similarly, the mean PDI score for the DR-CPR group was significantly lower than that of non-DR-CPR survivors (74.4 ± 19.9 vs. 85.1 ± 17.2; p = 0.027) as shown in figure 2. The proportion of significantly affected infants, with an MDI score ≤ 70, was 50 % in the DR-CPR group compared to 27 % in the infants who did not require DR-CPR (p = 0.045). The proportion of infants with a PDI score # 70 was 33 % vs. 21 % respectively (p = 0.227).
Figure 2.Univariate comparison of the Bayley II Mental and Psychomotor Developmental Index Scores at 18 Months Corrected Age.* p < 0.05.MDI (No DR-CPR 81.3 ± 17.7 vs. DR-CPR 67.7 ± 18.3; p = 0.006). PDI (No DR-CPR 85.1 ± 17.2 vs. DR-CPR 74.4 ± 19.9; p = 0.027).MDI, the Mental Developmental Index Score. PDI, the Psychomotor Developmental Index Score. DR-CPR, delivery room cardiopulmonary resuscitation.
Discussion
The literature is equivocal with regards to the effectiveness of DR-CPR in small premature infants. The results of this two-center cohort study demonstrate that DR-CPR is associated with higher mortality, with more short-term morbidity and is a predictor of worse neuromotor and cognitive outcome at 18 months.
In this study, we found that 13 % of infants born ≤ 1250 grams were treated with intubation, ventilation and cardiac compressions and/or epinephrine in the delivery room. Survival to discharge from the neonatal intensive care unit occurred for 60 % of infants who received delivery room resuscitation, which was significantly less than for infants who were not resuscitated (85 %). As expected, as the birth weight decreased, so did survival in both groups.
After adjusting for potential confounders, we found statistically significant differences in mortality and in combined poor short-term outcome in the group of infants born between 1,001 and 1,250 and in severe IVH in infants born between 751 and 1,000 grams.
As birth weight category decreased the trend of increased prevalence of poor short-term outcomes in infants requiring resuscitation is still present, but the differences are less striking and not significant. These findings may be related to the small sample size in infants with birth weight ≤ 750 grams (Type II error) but it may also be that at the border of viability the risk for poor short-term outcome secondary to extreme prematurity and/or the delivery process outweighs the risk associated with cardiopulmonary resuscitation in the delivery room.
To our knowledge this is the first study that compares long term neurodevelopmental outcomes between infants born ≤ 1,250 grams who underwent DR-CPR and those who did not. Prior studies have been limited to the description of few survivors and their long-term outcomes 13,14. The mean MDI and PDI scores were lower among those exposed to DR-CPR compared to the non-DR-CPR infants. The proportion of infants classified as significantly affected with an MDI score ≤ 70 was also higher in the DR-CPR group when compared to the infants that did not require such intervention, with poor skills such as imitation, vocalization and rudimentary problem solving. Finally, the proportion of significantly delayed infants in areas such as fine and gross motor skills (PDI) was higher among resuscitated infants but did not achieve statistical significance.
There are several limitations to this study. First is the retrospective nature of the design and the need to resort to chart review, although the data from our database and the long-term evaluation were collected prospectively and without any modification based on resuscitation measures, potential confounding variables were identified in this cohort study and statistical adjustment was performed by logistic regression modeling, when necessary. In addition infants classified as "resuscitated in the delivery room" may have had different duration and intensity of resuscitation requiring either chest compressions and epinephrine or only one of the measures. However, the definition of DR-CPR that lumps all infants that receive chest compressions and/or epinephrine is the most commonly used in the literature that has attempted to describe this important event and its consequences 7,13,14. We also acknowledge that the rate of follow up was not high and this may bias the results, as patients who do not return to follow up have been reported to over-represent the most affected infants 20. Conversely, infants who fail to follow up may actually have better outcomes than those who return for evaluation 21. In our study, infants born within the highest birth weight group category were less likely to return for neurodevelopmental assessment and follow up. Finally, the cohort in our study has only been assessed up to 18 months post conceptional age. It has been recently suggested 22 that results obtained at 18 months post conceptional age may have poor predictive validity in later follow up exams.
Conclusions
From our findings, we conclude that DR-CPR in infants with birth weight between 1,001 to 1,250 grams is a predictor for inpatient mortality and also for combined poor short-term outcome. Furthermore, DR-CPR is also a predictor for S-IVH among infants born between 751-1,000 grams. The magnitude of the risk for poor short-term outcomes associated with DR-CPR decreases as birth weight decreases. Additionally, among the infants who were evaluated at 18 months corrected age, DR-CPR was associated with worse neurodevelopmental outcome.
In summary, DR-CPR is an important perinatal risk factor that must be accounted and controlled for when analyzing and describing short and long term outcomes in very premature infants with birth weight < 1,250 grams. Additionally, if these findings and associations are replicated by other investigators in different clinical settings, the potential for poor short and long term outcomes associated with DR-CPR would need to be included in prenatal and postnatal discussions to provide more complete information to parents.
Acknowledgements
Supported in part by the Goddard Scholar, CRC, of Emory University (A.S.)
The authors would like to thank Ann Critz MD, George Bugg MD MPH, and Susie Buchter MD for their contribution to the clinical data, Linda Black MD, Ira Adams-Chapman MD, Maureen Larossa RN and Sheena Carter Ph D. for the developmental follow-up testing and follow-up data management and Mostafizur Rahman MBBS MPH for clinical database management.
Correspondence:
R. Deulofeut MD MPH.
4449 Mockingbird Lane.
Highland Park, TX 75205.
E-mail: richard_deulofeut@pediatrix.com