To assess attitudes, beliefs and knowledge of primary medical care professionals as regards the follow-up of Childhood Cancer Survivors (CCS) and the introduction of a Long-Term Follow-Up Program for Childhood Cancer Survivors in the Region of Murcia (PLASESCAP-MUR).
Material and methodsDescriptive cross-sectional study using a structured, self-administered questionnaire. These questionnaires were sent to all primary medical care professionals in Murcia Health District 1.
ResultsResponse rate of 58% (100/172), with 71% and 22% being family physicians and paediatricians, respectively, of whom 49% provided medical care to a CCS in the last 5 years, with 84% reporting that they never or rarely received a detailed report of overall assessment of the survivor. More than 75% found that access to detailed follow-up information was quite or very useful; 95% prefer to consult experts when providing medical care to survivors, and 80% believe that improving the quality of the environment may decrease the morbidity and mortality of the survivors. A statistically significant relationship was found between the length of practicing medicine and the perception of the importance of environmental factors.
ConclusionsIt seems to be important to increase the training of primary care professionals for the long-term follow-up of CCS, as well as having the detailed information through a personalised long-term follow-up of each survivor. PLASESCAP-MUR offers an integrated follow-up to CCS in a model of shared care between Long Term Monitoring Units and Primary Care Units.
Evaluar actitudes, creencias y conocimientos de los profesionales médicos de Atención Primaria acerca del seguimiento de los supervivientes de cáncer pediátrico (SCP) y divulgar el Programa de Largo Seguimiento de Supervivientes de Cáncer Pediátrico en la Región de Murcia (PLASESCAP-MUR).
Material y métodosEstudio transversal descriptivo mediante cuestionario estructurado y autocumplimentado. Se enviaron cuestionarios a todos los profesionales médicos de Atención Primaria del Área de Salud 1 del Servicio Murciano de Salud.
ResultadosTasa de respuesta del 58% (100/172). El 71 y el 22% eran médicos de familia y pediatras, respectivamente. El 49% atendió algún SCP en los últimos 5 años. El 84% refiere que nunca o pocas veces recibió un informe detallado de evaluación global del superviviente. Más del 75% encuentran bastante o muy útiles el acceso a información detallada de largo seguimiento. El 95% prefiere atender a los supervivientes conjuntamente con consulta de largo seguimiento. Un 80% considera que mejorando la calidad ambiental del entorno podría disminuir la morbimortalidad de los supervivientes. Se encontró una relación estadísticamente significativa entre años practicando medicina y percepción de importancia de algunos factores medioambientales.
ConclusionesPara el largo seguimiento de los SCP parece importante aumentar la capacitación de los profesionales sanitarios de Atención Primaria y la información detallada a través de un plan personalizado de largo seguimiento de cada superviviente. PLASESCAP-MUR proporciona un seguimiento integrativo a los supervivientes de cáncer pediátrico en un modelo de atención compartida entre la Unidad de Largo Seguimiento y Atención Primaria.
Any child with cancer is a childhood cancer survivor (CCS) from the time of diagnosis, and will continue to be one for the rest of his or her life.1 In Spain, approximately 950 children less than 15 years of age are diagnosed with cancer each year.2 In recent decades, their survival rate has increased spectacularly thanks to the progressive improvement in the available treatments, the creation of referral units in hospitals and international cooperation studies.3 The overall five-year survival rate for childhood cancer in the autonomous community of the Region of Murcia is approximately 80%, very similar to the rates for the whole of Spain (77% in the 2000–2003 period) and Western Europe (81% from 1995 to 2003).4,5 This increase in survival has brought forth the need to monitor for possible late relapses and the risk to develop subsequent neoplasms,6–8 chronic diseases and dysfunctions that affect quality of life at earlier ages than the general population.4,9,10 By the second decade of life, more than 60% of CCSs will suffer from at least one chronic disease related to the treatment they have received and/or associated environmental risk factors.11 This trend continues to rise during the life of the survivor, and by around 50 years of age more than 50% of CCSs will have experienced a severe or disabling life-threatening or fatal disease.12 National and international agencies recommend a structured and if possible lifelong follow-up of CCSs.4,13–15 Different models to guarantee the adequate follow-up of survivors are being considered. In the Region of Murcia, which has an established public primary care (PC) health system, we have developed a shared-care model for the transition from hospital care (long-term follow-up unit) to primary care (PC) that is tailored to the specific needs of each CCS. Most adult and some adolescent CCSs are followed-up by their primary care physicians (PCPs),15–17 and an appropriate transition from hospital to primary care is essential to guarantee the adequate long-term follow-up of CCSs. In Spain, the transition to PC is still performed in a mostly unstructured manner.18 The aims of this study were to: (a) assess the beliefs, attitudes and preferences of PC physicians regarding the follow-up of CCSs, and (b) explain the basic structure of the Childhood Cancer Survivor Long-Term Follow-up Programme of the Region of Murcia (Programa de Largo Seguimiento de Supervivientes de Cáncer Pediátrico en la Región de Murcia [PLASESCAP-MUR]).
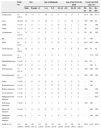
Materials and methodsWe conducted the study in Health Area 1 (Murcia/Oeste) of the Region of Murcia, which has a total population of 256725 inhabitants and a population under 15 years of age of 45302. Health Area 1 comprises 14 basic health zones (BHZs) each of which has a designated primary care centre. It has 38 paediatric clinics and 127 family medicine clinics. Table 1 shows the distribution of childhood cancer in Area 1 Murcia/Oeste over the 1998–2014 period. The PLASESCAP-MUR programme includes individuals diagnosed with cancer at ages less than 15 years since 1998.19 A total of 113 children were diagnosed with cancer in Area 1 during this period. In 2014, 32 (28%) of CCSs were older than 18 years of age. Inclusion in the long-term follow-up programme is granted to all patients that received a cancer diagnosis during childhood if three or more years have elapsed since the end of treatment and they have remained disease-free. Table 2 shows the structure and questionnaires of the PLASESCAP-MUR.20–27 Prior to implementing the PLASESCAP-MUR training activities in the PC setting, questionnaires were sent to the medical coordinator of each of the 14 BHZs for their distribution to the 172 physicians. Of these physicians, 71% were family physicians, 22% paediatricians and 7% resident physicians. The self-administered questionnaire had a structured format and assessed the attitudes, preferences and beliefs of PC family physicians and paediatricians concerning the follow-up of CCSs.28–30 The questionnaire, which is available on the PLASESCAP-MUR website,20 consists of 13 questions about the follow-up of CCSs: demographic characteristics, medical training and professional characteristics of the providers. Physicians were asked whether they had cared for any CCSs in the past five years and how often they had been given a detailed report or personalised long-term follow-up plan (diagnosis, types of treatment and dosages, identified risks, late effects), measured on a 5-point Likert scale ranging from 1 (never) to 5 (always). A similar scale was used to measure their level of comfort in caring for CCSs, from 1 (very uncomfortable) to 5 (very comfortable) and their familiarity with the existing guidelines for the long-term follow-up of CCSs, ranging from 1 (not at all familiar) to 5 (very familiar). Physicians were also asked about their preferences for the care of CCSs (referral to a different level of care, independent care offered by the physician, or shared care with the long-term follow-up clinic). They were asked about the usefulness of four tools that may improve the care of CCSs (detailed report, long-term follow-up guidelines, continued education and communication by telephone or electronic mail with the long-term follow-up clinic), using the same type of scale ranging from 1 (not at all useful) to 5 (very useful). Finally, they were asked whether improvements in environmental quality would reduce morbidity and mortality in CCSs on a scale from 1 (strongly disagree) to 5 (strongly agree) and to rate how different environmental risks can affect CCSs on a scale from 1 (very little) to 4 (to a great extent). We performed descriptive and regression analyses to assess the possible correlation between qualitative variables and the number of years the physician had been practising medicine. The confounding variables selected a priori were sex and the number of patients seen per week. We performed all the statistical analyses with the SPSS software version 15.0 (SPSS Inc., Chicago, USA).
Childhood cancers in Health Area 1 (Murcia/Oeste) by type of tumour, sex, age, subperiod and survival rate.
| Total (%) | Sex | Age at diagnosis | Age of survivors in 2014 | 5-year survival rate (%) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Male | Female | <1 | 1–4 | 5–9 | 10–14 | <10 | 10–18 | >18 | 98–01 | 02–05 | 06–09a | ||
| Leukaemias | 33 (29.2) | 16 | 17 | 1 | 19 | 8 | 5 | 11 | 17 | 5 | 83.3 | 100 | 87.5 |
| ALL | 26 (23) | 14 | 12 | 0 | 18 | 5 | 3 | 9 | 15 | 2 | 100 | 100 | 80 |
| AML | 4 (3.5) | 2 | 2 | 1 | 1 | 2 | 0 | 2 | 1 | 1 | 50 | – | 100 |
| Other | 3 (2.7) | 0 | 3 | 0 | 0 | 1 | 2 | 0 | 1 | 2 | 50 | – | 100 |
| Lymphomas | 14 (12.4) | 11 | 3 | 0 | 2 | 3 | 9 | 1 | 4 | 9 | 50 | 80 | 100 |
| HL | 4 (3.5) | 3 | 1 | 0 | 0 | 1 | 3 | 0 | 1 | 3 | 0 | 100 | – |
| NHL | 10 (8.9) | 8 | 2 | 0 | 2 | 2 | 6 | 1 | 3 | 6 | 66.7 | 66.7 | 100 |
| CNS tumours | 23 (20.3) | 14 | 9 | 1 | 7 | 10 | 5 | 7 | 8 | 8 | 100 | 75 | 50 |
| Astrocytoma | 11 (9.7) | 5 | 6 | 0 | 4 | 6 | 1 | 3 | 7 | 1 | – | 71.4 | 100 |
| Medulloblastoma | 5 (4.4) | 4 | 1 | 0 | 2 | 2 | 1 | 1 | 0 | 4 | 100 | 50 | – |
| Other | 7 (6.2) | 5 | 2 | 1 | 1 | 2 | 3 | 3 | 1 | 3 | – | 100 | 0 |
| SNS tumours | 15 (13.3) | 9 | 6 | 11 | 2 | 1 | 1 | 9 | 5 | 1 | 100 | 100 | 100 |
| Neuroblastoma | 14 (12.4) | 8 | 6 | 11 | 2 | 1 | 0 | 9 | 5 | 0 | 100 | 100 | 100 |
| Other | 1 (0.9) | 1 | 0 | 0 | 0 | 0 | 1 | 0 | 0 | 1 | – | 100 | – |
| Retinoblastoma | 2 (1.8) | 1 | 1 | 1 | 1 | 0 | 0 | 1 | 1 | 0 | – | 100 | – |
| Kidney tumours | 3 (2.7) | 1 | 2 | 0 | 2 | 1 | 0 | 1 | 1 | 1 | 100 | – | 100 |
| Liver tumours | 2 (1.8) | 1 | 1 | 2 | 0 | 0 | 0 | 2 | 0 | 0 | – | – | 100 |
| Malignant bone tumours | 4 (3.5) | 2 | 2 | 0 | 1 | 1 | 2 | 1 | 1 | 2 | – | – | 66.7 |
| Soft tissue sarcomas | 7 (6.2) | 4 | 3 | 3 | 2 | 1 | 1 | 2 | 5 | 0 | 100 | 100 | – |
| Stem cell tumours | 5 (4.4) | 1 | 4 | 0 | 0 | 3 | 2 | 0 | 2 | 3 | – | 100 | 100 |
| Malignant epithelial tumours | 5 (4.4) | 4 | 1 | 0 | 0 | 1 | 4 | 0 | 2 | 3 | – | 100 | 100 |
| Total, n (%) | 113 (100.0) | 64 (56.6) | 49 (43.3) | 19 (16.8) | 36 (31.8) | 29 (25.6) | 29 (25.6) | 35 (30.9) | 46 (40.7) | 32 (28.3) | 88.9 | 94.4 | 89.4 |
ALL, acute lymphoblastic leukaemia, AML, acute myeloblastic leukaemia; CNS, central nervous system; HL, Hodgkin lymphoma; NHL, non-Hodgkin lymphoma; n, number of cases; SNS, sympathetic nervous system. Grouped according to the International Classification of Diseases for Oncology (ICD-O-3) and the International Classification of Childhood Cancer.
Structure of long-term follow-up care and questionnaires of the PLASESCAP-MUR.
| Environmental medical history of childhood cancer survivor | ||
| At the time of diagnosis | HVERDE: green sheet for environmental screening, including personal data, disease classification, age at diagnosis, smoking, chemical exposure risk involved in the parents’ occupation, geographical location and aetiological risk perception of parents | |
| ≥3 years after the end of cancer treatment and being disease-free | HTRANSI | Transition to long-term follow-up care sheet. Explanation about the PLASESCAP and of the importance of long-term follow-up |
| Risk factors | Descriptive questionnaire about prenatal and postnatal risk factors described in the scientific literature as having an association with the development of each type of tumour. It includes environmental and familial risk factors, including the cancer history of at least three generations, the presence of genetic and constitutional factors associated with childhood cancers, presence of chronic, rare and/or inherited diseases, and causes of death. | |
| Treatment | Detailed report of the treatment, including types of treatment and dosages used | |
| Late effects | Identification of potential late effects based on the treatment received and recommended follow-up | |
| Environmental quality and quality of life | Questionnaires on environmental quality (smoking and other legal and illegal drugs, physical activity, contact with nature, healthy diet, sun protection, use of pesticides and other chemical products, risk of exposure in the workplace, social risks, environmental risks in the house/community, and radiation protection). Administration of the PedsQL™ questionnaire, which assesses quality of life aspects in physical activity, mood, social relationships and academic activities | |
| Long-term follow-up plan | Summary including the recommendations for the screening/monitoring of late effects and specific preventive measures through an improvement plan based on the identification of personal risk factors | |
| Hard copies of the report given to the survivor and his/her parents, copy submitted to the survivor's primary care physician | ||
| Follow-up | Yearly or every two years, shared care by long-term follow-up unit and primary care | |
All the BHZs agreed to participate in the study. We received 100 questionnaires out of the 172 that had been sent out (response rate, 58.1%). The response rate was slightly higher among paediatricians than among family physicians (60.5% vs. 55.1%; P=.9). Of all respondents, 49.4% reported having seen at least 1 CCS in the 5 years preceding completion of the questionnaire. Table 3 summarises the demographic and professional characteristics of the participating physicians. Eighty-four percent reported that they had never or rarely (Likert scale score ≤2) received a detailed report or personalised long-term follow-up plan (diagnosis, type and dosage of treatments, identified risks, late effects) for CCSs. Only 34.0% of the surveyed physicians reported feeling “comfortable” or “very comfortable” (Likert scale score ≥4) providing care for CCSs. Ninety-five percent preferred to care for CCSs in collaboration with the long-term follow-up clinic, while none of the respondents preferred being solely responsible for their follow-up.
Demographic and healthcare characteristics of participating physicians.
| Characteristics | Frequency (%a) |
|---|---|
| Sex | |
| Male | 39 (39) |
| Female | 61 (61) |
| Total | 100 (100) |
| Years practising medicine, mean±SD=23.19±9.3 | |
| ≤18 | 27 (29) |
| 19–24 | 20 (22) |
| 25–31 | 27 (29) |
| 32+ | 19 (20) |
| Total | 93 (100) |
| Patients seen/week, mean±SD=215±58 | |
| ≤160 | 19 (20) |
| 161–200 | 29 (31) |
| 201–225 | 11 (12) |
| 226–260 | 16 (17) |
| 261+ | 18 (19) |
| Total | 93 (100) |
| Category/specialty | |
| Family and Community Medicine | 71 (71) |
| Paediatrics | 22 (22) |
| Family and Community Medicine resident | 7 (7) |
| Total | 100 (100) |
| Have you seen a CCS in the past five years? | |
| Yes | 44 (49) |
| No | 45 (51) |
| Total | 89 (100) |
CCS, childhood cancer survivor.
Of all respondents, 37.1% was familiar with the long-term follow-up guidelines for CCSs (Likert scale score, 1.5). Table 4 shows the perception of clinicians regarding the usefulness of different tools used in the follow-up of CCSs. More than 80% of the surveyed PC physicians considered that generally speaking, the different resources used to improve the quality of the follow-up of CCS (detailed report, long-term follow-up guidelines, continuing education and direct contact with the long-term follow-up clinic) were quite or very useful (Likert score ≥4).
Perception of the usefulness of several tools for improving the care of CCSs.
| Perception | Not at all useful | Somewhat useful | Useful | Quite useful | Very useful |
|---|---|---|---|---|---|
| UID (%) | 1 (1) | 0 (0) | 7 (7) | 23 (24) | 64 (67) |
| UAG (%) | 1 (1) | 3 (3) | 11 (11) | 31 (32) | 50 (52) |
| UCE (%) | 1 (1) | 2 (2) | 15 (16) | 29 (30) | 49 (51) |
| UTC (%) | 0 (0) | 1 (1) | 5 (5) | 26 (27) | 64 (67) |
UAG, usefulness of access to guidelines; UTC, usefulness of telephone contact; UCE, usefulness of continuing education; UDR, usefulness of detailed report.
Percentages: the values represented as percentages do not include missing values unless so noted.
Of all respondents, 80.2% strongly agreed or agreed (Likert scale score ≥5) that improving environmental quality could reduce the morbidity and mortality of CCSs. They expressed that the environmental risks that affect CCSs most often are (Table 5): exposure to pesticides (mean, 3.74), environmental smoke (mean, 3.67), ionising radiation (mean, 3.62), outdoor air pollution (mean, 3.62) and legal or illegal drug use (mean, 3.53). We found a significant association between the number of years physicians had been practising medicine and the importance they attributed to the impact of environmental factors on CCSs, such as a lack of contact with nature, the state of the living setting, the use of legal and illegal drugs, exposure to second-hand smoke and sedentary lifestyles.
Perception of the effect of environmental risk factors on the morbidity of CCSs.
| How strong is the effect of… | Score (on a 1–4 scale)a | Has a “very strong” effect 4/4 (% of participants) |
|---|---|---|
| Legal and illegal drug use | 3.53 | 62 |
| Passive smoking | 3.67 | 70 |
| Sedentary lifestyle | 2.85 | 19 |
| Diet poor in fresh fruits and vegetables | 3.34 | 47 |
| Little contact with nature | 2.77 | 14 |
| Exposure to pesticides | 3.74 | 79 |
| Outdoor air pollution | 3.62 | 66 |
| State of living setting | 2.90 | 18 |
| Exposure to toxic substances | 3.42 | 52 |
| Ultraviolet radiation | 3.40 | 54 |
| Ionising radiation | 3.62 | 65 |
To our knowledge, this is the first study conducted in Spain that analyses the attitudes, knowledge and preferences of PC physicians concerning the follow-up of CCSs. Furthermore, we asked PC physicians about the association between environmental risks and the morbidity and mortality of CCSs. Most of the physicians (80%) strongly agreed or agreed that improving environmental quality would succeed in reducing the morbidity and mortality of CCSs, and identified the environmental risks that affect them most: exposure to pesticides, exposure to environmental tobacco smoke, ionising radiation, outdoor air pollution and use of legal/illegal drugs. Several studies have emphasised the need for lifestyle changes and reducing or eliminating the environmental risks as being among the most important goals in the long-term follow-up of CCSs.3,31,32 Chief among the findings in our study was that 84% of the surveyed physicians stated that they had never or rarely received a detailed report from the oncology centre presenting not only the diagnosis and general aspects of the treatment, but also a personalised risk assessment and long-term follow-up plan. We believe that this report or survivorship care plan constitutes a fundamental pillar around which to build a quality long-term follow-up,3,33 and so do physicians, of whom 91% considered that it was quite useful or very useful. The basic elements of such a plan include a summary of the treatments received, information on the potential late effects that may develop, and recommendations for follow-up.34,35 Having a personalised care plan increases the probability of patients receiving adequate follow-up care and does not increase their worry about cancer.30,33 These data are similar to those of other studies conducted in the United States, where the use of care plans for CCSs was low (<20%) but PC physicians considered them very useful (>90%).29
Another salient finding is that 66% of physicians reported feeling somewhat uncomfortable or uncomfortable treating CCSs and 95% preferred to care for them in collaboration with a specialised long-term follow-up unit. Their discomfort in treating CCSs could be related to a lack of experience in the follow-up of survivors by professionals in the PC setting. Nathan et al.28 found similar results in their study, in which 85% of respondents preferred caring for CCSs in collaboration with oncologists or in the context of a long-term follow-up programme.
Previous studies have shown that CCSs are at greater risk of morbidity and mortality during childhood, adolescence and adulthood, usually due to late relapses, secondary tumours and an increased susceptibility to the early development of chronic diseases of adulthood.36,37 This makes CCSs a particularly vulnerable group, and consequently it is very important to ensure an adequate long-term follow-up of these patients, preferably for life.4,13–15 Ideally, follow-up would extend to the children and grandchildren of CCSs. In Spain, as in most western countries, long-term follow-up programmes for CCSs are being set up.38 Patients are mostly followed-up by oncologists and haematologists that treat the primary disease and perform the follow-up for a variable and increasingly long period of time. Sooner or later, patients are discharged from these services and transferred to PC, where paediatricians or family physicians will be their primary care providers and be responsible for their follow-up.3,15–17 The province-based organisation of care provision and the prior experience of two referral units, the Unidad de Salud Medioambiental Pediátrica of Murcia (Unit of Paediatric Environmental Health [PEHSU]) and the Unidad de Oncología y Hematología Pediátricas (Paediatric Oncology and Haematology Unit) of the Hospital Clínico Universitario Virgen de la Arrixaca, has allowed the launching of an integrated long-term follow-up programme. In the PLASESCAP-MUR programme, patient care and follow-up are based on the individual needs of each patient. The programme is carried out by the long-term follow-up clinic and PC services in a shared care model.39 Thus, as the programme continues to develop, PC paediatricians, family physicians and nurses will be increasingly engaged in the follow-up of CCSs. One of the goals of the PLASESCAP is education in, and the promotion of, healthier environments and lifestyles for the survivor, his or her family and the community, in order to improve their environmental quality and quality of life. Another goal is the performance of screenings for the early detection and appropriate management of late effects of the disease and the treatments received by the patient.20 The PLASESCAP will address a good portion of the needs identified through the questionnaire, promoting access to quality reports for the long-term follow-up of each CCS and increasing the skills of PC healthcare professionals in the management of CCSs. One of the limitations of this study is the low response rate (58.1%), although it was higher than response rates in similar studies in PC settings (which range between 23% and 45%)28,29 and similar to the 61% response rate for questionnaires administered to hospitalists.30 The low response rate may have been due to the lack of knowledge on this topic of providers in this BHZ. The questionnaires were collected prior to a clinical training session on CCSs and a second round could not be administered, as we believed that the responses could have been biased after the session, and we were unable to analyse the characteristics of nonrespondents. On the other hand, while the sample was small, it was representative of the Health Area, as it included all of its physicians. Last of all, since our findings are based on the perceptions of PC physicians, they may not reflect what actually occurs in clinical practice.
Using the resources available through the national health system of Spain, with its high coverage, quality, and focus on prevention through PC, to develop long-term follow-up programmes, could offer better health options to this subset of the population.
FundingThis study was funded partially by the Plan de Formación Continuada (Continuing Education Programme) of the Health Area 1 of Murcia Oeste, Servicio Murciano de Salud (Murcia Health Service), training action n. I-14-10184-14, and the grant MD 001452 IP: Dr. Luz Claudio, National Center on Minority Health and Health Disparities of the National Institutes of Health.
Conflicts of interestThe authors have no conflicts of interest to declare.
The authors want to thank all childhood cancer survivors and their families for their generous contribution, and all the primary care professionals for their collaboration and enthusiasm in the performance of this study.
Please cite this article as: Cárceles-Álvarez A, Ortega-García JA, Fuster-Soler JL, Rivera-Pagán GA, Bermúdez-Cortés M, Gomariz-Peñalver V, et al. Programa de largo seguimiento de supervivientes de cáncer pediátrico en la Región de Murcia: preferencias y actitudes de los profesionales de Atención Primaria. An Pediatr (Barc). 2015;83:264–271.