The ability to perform magnetic resonance imaging (MRI) without sedation in the neonatal period increases patient safety, availability and profitability of the diagnostic tool. The aim in this study was to evaluate a new protocol of MRI without sedation during a 20-month period. In the protocol, the patients are prepared in the neonatal unit.
Patients and methodProspective descriptive study, from May 2012 to December 2013. Patients included were neonates requiring MRI, clinically stable and not requiring ventilatory support. The method was based on the application of developmental centred care and the use of a vacuum mattress to immobilise the baby. The principal outcome parameter of interest was the percentage of successfully completed MRIs. The duration of the MRI and the number of interruptions, was also studied from October 2012.
ResultsA total of 43 MRIs without sedation were carried out on 42 patients: 41 cerebral and 2 spinal. The success rate was 97.7% (42/43). The mean MRI time was 26.3min (95% CI 23.3–29.3min; range 16–50min). MRIs were completed without interruption in 20 of the 34 cases (58%) in which the duration was recorded. The number of interruptions per procedure varied from 0 to 3, with a mean of 0.6 (95% CI 0.3–0.8) and a median of 0.
ConclusionThe protocol had a success rate of over 90%. Thus MRI without sedation seems applicable in Spanish hospitals, with most of the preparation being performed in the neonatal unit, in order to reduce the occupation of the MRI unit, as well as minimising stress to the baby.
La posibilidad de llevar a cabo RM sin sedación en el período neonatal aumenta la seguridad del paciente, la disponibilidad y rentabilidad de la prueba. El objetivo fue describir la experiencia de 20 meses con el nuevo protocolo de RM sin sedación, en el que la preparación del paciente se realiza en la unidad neonatal.
Pacientes y métodoEstudio descriptivo prospectivo, de mayo del 2012 a diciembre del 2013. Los pacientes incluidos fueron neonatos con indicación de RM, estables y sin soporte ventilatorio. El procedimiento se fundamentó en la aplicación de cuidados centrados en el desarrollo y el uso de un colchón de vacío como sistema de inmovilización. La variable resultado principal fue el porcentaje de RM completadas con éxito. Desde octubre del 2012 se recogieron además la duración de la prueba y el número de interrupciones.
ResultadosSe llevaron a cabo 43 RM sin sedación, 41 cerebrales y 2 de columna vertebral. La tasa de éxito fue del 97,7% (42/43). La media de tiempo de RM fue 26,3min (IC del 95%, 23,3–29,3min; rango 16–50min). Se completó la prueba sin interrupciones en 20 de los 34 casos (58,8%) en los que se recogió este dato. La media de interrupciones fue 0,6 (IC del 95%, 0,3–0,8; rango 0–3) y la mediana 0.
ConclusionesEl protocolo tuvo una tasa de éxito superior al 90%. Por tanto, la RM sin sedación parece factible en nuestro medio, realizando gran parte de la preparación en la unidad neonatal para así disminuir la ocupación de la sala de RM.
The use of magnetic resonance imaging (MRI) in the neonatal period has increased in recent years, partly due to the growing concern with the neurologic prognosis of premature or severely ill newborns (NBs). Until a few years ago, it was considered necessary to sedate or anaesthetise NBs that were going to be subjected to an MRI scan to avoid motion artefacts and obtain images with good quality. But this practise involves exposing the patient to the risks associated with sedative or anaesthetic drugs, a decrease in the availability of the test, an increase in healthcare costs and the need for time-consuming monitoring of the patient following the examination.1–3 The possibility of performing MRI without sedation or anaesthesia (MRWS) in the neonatal period increases the safety of the patient as well as the availability and the cost-effectiveness of the test, which allows for expanding its indications.4,5
Few studies have been published on the subject, but they all show excellent results, as they reported the acquisition of images of good quality in a high percentage of the tests4–8 and demonstrated that the procedure is safe in term NBs as well as preterm NBs if the scan is performed at term-equivalent age.4,9,10
Protocols to perform MRWS in the neonatal period have been described in detail.1,4,6 Most authors use a vacuum mattress for immobilising the NB in order to reduce the appearance of motion artefacts.1,4–7,9
In light of the good results reported by other centres, we decided to form a multidisciplinary team and launch our own MRWS protocol. The aim of this study was to describe our 20-month experience with the new MRWS protocol, which specifies that the preparation of the patient be carried out in the neonatal unit.
Patients and methodsWe conducted a descriptive prospective study from May 2012 to December 2013. Before the study started, we developed a MRWS protocol that involved the use of a vacuum mattress (BPOD2-002 vacuum mattress fitted with an exothermic mattress compatible with the BabyPod II EVO4, Adaro Tecnología S.A., Gijón, Spain) to immobilise the NB.
In the 4 months preceding the implementation of the MRWS protocol, we formed a multidisciplinary team consisting of a paediatric neurologist, a paediatric neuroradiologist, and a neonatologist from our centre. We reviewed the literature, and the principal author gained practical experience at the Erasmus Medical Centre-Sophia in Rotterdam, the Netherlands. We developed the MRWS protocol and offered educational workshops in the paediatrics and neonatology departments attended by paediatricians, paediatric neurologists and radiologists.
The inclusion criteria for the MRWS protocol were: NB in whom MRI is indicated, clinically stable and not requiring ventilatory support.
The primary endpoint was the percentage of MRI attempts completed successfully. Success was defined as achieving images of the same quality as images obtained up to that point in MRI studies with sedation, allowing the interpretation of all the requested and performed sequences. From October 2012, we also documented the duration of the procedure and the number of interruptions required during it. The duration of the procedure was defined as the time elapsed from the moment the child entered the MRI room to the time the scan was considered done, expressed as mean and confidence interval. Any adverse events were documented in writing.
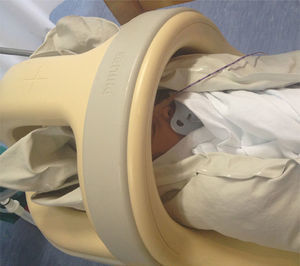
ProcedureBefore the MRI scan was performed we obtained the consent of the parents and invited them to accompany the child during the procedure. We scheduled the special care required on the day of the test with the nursing staff, with the reminder that the child could not wear anything made of metal and that feedings needed to be adjusted so that the child would feed approximately 30min before the test. The preparation for the test was performed in the neonatology department, trying to make the NB as comfortable as possible. Ear protection was placed carefully (Macks Hot Orange Child Size Pillow Soft Silicone Ear Plugs, McKeon Products, Inc., Michigan, USA; and Algo Supplies, Natus Medical, Inc., California, USA), the pulse oximeter probe was placed on the foot to facilitate access, the NB was swaddled in sheets, fed before transfer, and was laid on the vacuum mattress in the cot to encourage sleep. The NB was transferred to the neuroradiology department while monitored by pulse oximetry, and placed in the neonatal MRI unit. Once there, the air was removed from the mattress by attaching a suction device to the valve included on the side of the mattress for that purpose. As the air was evacuated, the mattress was fitted manually around the head and neck of the NB to ensure that this area was properly immobilised (Fig. 1). Then a blanket was placed covering the body of the NB. When everything was ready, the patient was slid into the scanner and the procedure started. The images were captured with a 1.5T MRI unit (Achieva 1.5T A-series, Philips Healthcare, Eindhoven, The Netherlands). During the scan, the NB was monitored by pulse oximetry. If there were changes in the vitals or motion artefacts in the images, the scan was interrupted, the NB was examined, and an attempt was made to solve the problem in order to continue. When the test was completed, air was allowed back into the mattress, which then became softer, and the NB was removed from the scanner and placed back on the cot. Later on, the NB was transferred back to the neonatology department and the physician in charge filled out the data collection sheet for future analysis.
A physician (neonatologist or paediatric resident), a neonatology nurse and the parents, if they so willed, were present during the entire procedure (preparation, transfers, and resonance).
Statistical analysisWe performed a descriptive analysis of the characteristics of the NBs included in this study. We calculated the success rate of MRI without sedation: (number of successful MRWS/total number of attemped)×100.
We assessed the normality of the distribution of the variables under study by means of the Kolmogorov–Smirnov test. We have expressed qualitative variables as absolute frequencies and percentages, and quantitative variables as mean, 95% confidence interval (CI) for the mean, and range. We calculated the median for non-normally distributed variables.
We studied three variables over two time periods (October 1, 2012 to May 31, 2013 and June 1, 2013 to December 31, 2013), searching for differences between both periods to assess whether the results improved with time. The variables were the type of physician in charge of preparing the NB (attending vs. resident), the duration of the MRWS, and the number of interruptions needed during the MRWS. We also compared the duration of MRWS in relation to whether interruptions had been needed or not. We used the chi square test to compare categorical variables, the Mann–Whitney U test for non-normally distributed quantitative variables, and Student's t test for normally distributed quantitative variables. Differences were considered significant for P<0.05. We performed all analyses using the software Statgraphics Centurion XVI version 16.1.15 (Statpoint Technologies, Inc., Warrenton, USA).
ResultsAll parents to whom we proposed performing MRWS on their children, accepted. From May 2012 through December 2013 a total of 43 MRWS were performed on 42 patients, of which 21 were male (50%), 28 term NBs, and 14 preterm NBs. Of the 43 MRWS scans, 41 were of the brain and 2 of the spine. The weight and gestational age characteristics of the patients are shown in Table 1. Table 2 shows the diagnoses of the patients that underwent MRWS. The success rate of MRWS was 97.7% (42/43).
Characteristics of newborns subjected to magnetic resonance without sedation (n=43).
| Variable | Mean (95% CI) | Range |
|---|---|---|
| GA | 36 weeks (34–37) | 24–41 weeks |
| Birth weight | 2509g (2185–2832) | 600–4250g |
| Days of life at the time of MR scan | 27 days (17–36) | 2–102 days |
| CGA at the time of MR scan | 40 weeks (39.5–40.7) | 36–45 weeks |
CGA, corrected gestational age; CI, confidence interval; GA, gestational age; g, grams; MR, magnetic resonance.
Diagnoses of newborns subjected to magnetic resonance without sedation (n=43).
| Diagnosis | Number of MR | Type of MRWS | ||
|---|---|---|---|---|
| PTNBs | Brain damage detected during ultrasound followup | 11 | P1: 6 | Brain |
| P2: 3 | ||||
| Congenital infection by CMV | 1 | P1: 1 | ||
| P2: 0 | ||||
| Suspected malformation syndrome | 1 | P1: 1 | ||
| P2: 0 | ||||
| Epidural seizures | 1 | P1: 0 | ||
| P2: 1 | ||||
| TNBs | Moderate–severe HIE | 10 | P1: 3 | Brain |
| P2: 3 | ||||
| Epidural seizures | 5 | P1: 3 | ||
| P2: 2 | ||||
| Prenatal brain damage | 3 | P1: 1 | ||
| P2: 2 | ||||
| Venous sinus thrombosis | 2 | P1: 0 | ||
| P2: 2 | ||||
| Congenital infection by CMV | 2 | P1: 0 | ||
| P2: 1 | ||||
| Tuberous sclerosis | 1 | P1: 0 | ||
| P2: 1 | ||||
| Midline craniofacial malformations | 1 | P1: 0 | ||
| P2: 1 | ||||
| Hypotonia | 1 | P1: 1 | ||
| P2: 0 | ||||
| Suspected malformation syndrome | 1 | P1: 0 | ||
| P2: 1 | ||||
| Mild HIE | 1 | P1: 0 | ||
| P2: 1 | ||||
| Presacral teratoma | 1 | P1: 1 | Spine | |
| P2: 0 | ||||
| Spinal dysraphism | 1 | P1: 1 | ||
| P2: 0 | ||||
Diagnoses of all NBs subjected to MRWS since May 2012. Period 1 went from October 1, 2012 to May 31, 2013, and period 2 went from June 1, 2013 to December 31, 2013.
CMV, cytomegalovirus; HIE, hypoxic-ischaemic encephalopathy; MR, magnetic resonance; MRWS, magnetic resonance without sedation; NBs, newborns; P1, period 1 (Oct-1-12 to May-31-13); P2, period 2 (Jun-1-13 to Dec-31–13); TNBs, term newborns; PTNBs, preterm newborns.
From October 2012 through the end of the study 34 MRWS were performed. The mean duration of the MRI room use when MRWS was performed was of 26.3min (95% CI, 23.3–29.3min; range, 16–50min). The test was completed without interruptions in 20 out of the 34 procedures (58.8%) in which this data was collected. The mean number of interruptions was 0.6 (95% CI, 0.3–0.8; range, 0–3) and the median number was 0. In the 14 instances in which there were interruptions during the MRWS, the documented reasons for the interruptions were motion artefacts or changes in the heart rate or oxygen saturation due to restlessness or crying of the NB (73%) or to poor signal capture by the pulse oximetry probe (27%). The problems were resolved and the procedure was resumed and completed successfully in all instances but one (95%). The only instance in which the MRWS was not completed successfully was due to motion artefacts secondary to epileptic seizures at the time of the test. In this patient, the test was repeated under anaesthesia.
The median duration for MRWS procedures completed without interruption was 25min, and 30min for procedures in which there were interruptions (P=0.0766).
The physician in charge of preparing the NB for the MRWS was an attending neonatologist in 73.5% of the procedures (25/34) and a paediatric resident in 26.5% (9/34).
There were no adverse events.
We compared the duration of MRWS, the number of interruptions, and the type of physician in charge of the preparation of the NB in the two time periods (Table 3) to assess whether the results improved over time.
Comparison of the duration of magnetic resonance without sedation, number of interruptions, and physician in charge of preparing the newborn in two periods.
| Period 1 (Oct-1-12 to May-31-13) | Period 2 (Jun-1-13 to Dec-31-13) | P | |||||
|---|---|---|---|---|---|---|---|
| Duration (min) | Mean (95% CI) | Range | Mean (95% CI) | Range | 0.218 | ||
| 24.3 (19.9–28.8) | 20–50 | 28 (23.7–32.3) | 16–45 | ||||
| Interruptions (n) | Median | Mean (95% CI) | Range | Median | Mean (95% CI) | Range | 0.0505 |
| 0 | 0.2 (0.01–0.5) | 0–1 | 1 | 0.8 (0.3–1.3) | 0–3 | ||
| % MRWS with interruption(s) | 25% | 56% | 0.0708 | ||||
| Physician in charge | Attending 94% | Attending 56% | 0.033 | ||||
| Resident 6% | Resident 44% | ||||||
CI, confidence interval; min, minutes; MRWS, magnetic resonance without sedation.
Our study shows that it is possible to perform MRWS in clinically stable NBs with a high success rate (97.7%) thanks to the implementation of a protocol developed through the consensus of the different professionals involved in performing MRI. The protocol for the procedure was based mostly on the application of basic concepts of developmental care and the use of a vacuum mattress to ensure the immobilisation of the NB during the scan. The success rates of MRWS achieved in other countries with similar procedures have been comparable (92.8–100%).4,6–8 As described in other studies,8 no adverse events occurred when our new MRWS protocol was implemented.
Introducing MRWS should neither obstruct the workflow of the MRI room nor reduce the test's availability. In theory, the availability of the MRI room could increase if MRWS were performed instead of MR under sedation or anaesthesia, as in MRWS all the preparation can be done outside the scanning room, whereas the induction of anaesthesia is usually performed inside of it. However, we must take into account that a considerable percentage of procedures may require halting the process to soothe the child before resuming, which increases the duration of MRI. Nevertheless, a study in which cardiovascular MRI was performed, compared the duration of the scan and the total time inside the MRI room when sedation or anaesthesia were not used, and when sedation or general anaesthesia were used, and found that both times were shorter for MRWS.5 This comparison has not been made for brain MRI.
In our study, the mean duration of the MRWS session was 26.3min (95% CI, 23.3–29.3min), lower than the duration published by Neubauer et al. This author reported a mean duration of MRWS sessions of 36±14min. This difference may be due to the fact that in their study the NB was swaddled inside the MRI room, while in ours the NB was swaddled in the neonatal unit, so we propose that all preparations be performed outside the MRI room and that the minimum necessary be carried out in the latter to improve the availability of the test. Other authors have previously proposed doing all possible preparations in the neonatal unit, but had not measured the total time spent in the MRI room.1,4
In our experience, we had to interrupt the scan 41.2% of the time. The mean duration of the session was longer when interruptions were necessary compared to MRSW that were completed without interruptions, but this difference was not statistically significant. However, the need for interruptions did not affect the success of the test in any relevant way, as the problem was resolved in 95% of instances and the MRI scan could be resumed and completed successfully. In the study by Neubauer et al., 69.6% of the NBs underwent scanning without the need for interruptions, and the need for interruptions significantly increased the total time spent in the MRI room.6 Another study achieved a success rate of 100% in different imaging tests without sedation and without interruptions in any of the tests7 using an immobilisation system similar to ours.
When we compared the two periods in our study we found a trend towards longer duration in MRWS and a greater number of interruptions in the second period, despite having had a few months of experience with it. During the second period, there was a higher percentage of tests in which the doctor in charge of the preparation and transport of the NB was a resident. Given that we had good results with the MRWS protocol from the outset and that it was adding to the workload of attending physicians, the task was gradually delegated to resident physicians. Although a causal relationship has not been established, improving the training of resident physicians could increase the cost-effectiveness of this test by decreasing the total time spent in the MRI room. However, we cannot rule out that other factors that we did not study may have contributed to the differences we found, such as, for example, an asymmetrical distribution of the pathology of the NBs subjected to MRWS in the two time periods under study.
The strength of this study is that we obtained MRIs without using medication. This is particularly relevant considering that the pharmacokinetics or indication in the neonatal period of most drugs used on NBs are not well known. While MRI studies are not usually refused in clinical practise, the use of sedation may upset and concern parents. On the other hand, MRWS facilitates the use of this technique for examination in research studies in which the need of sedation could make the study ethically questionable and pose a barrier to obtaining the consent of parents.
The main limitation of this work is that we did not conduct a double-blind controlled study to assess and compare the quality of MRI images attempted with and without sedation or anaesthesia. In the absence of such a design, the presence of several examiners or an external evaluator would have increased the strength of the evidence. The procedure we have described has been successful in our centre, which carries out conventional MRI scans, but it would be convenient to investigate whether results are also satisfactory in more complex MRI studies, such as those including volumetry and tractography. Another potential disadvantage of this protocol is the need to reschedule patients for whom it has not been possible to achieve a quality MRWS, something that hospitals with high caseloads might want to take into consideration. Still, this only happened in one patient of our cohort, and in our experience, the availability of MRI increased after the implementation of the MRWS protocol.
Since Mathur et al. first published the instructions to avoid sedation during brain MRI in newborns,1 it has been demonstrated that they can be applied to centres without previous experience with very good results.6 At present, its use has been extended to perform MRWS of other body parts (spinal cord, abdomen, chest, pelvis and full-body)4,5,8 and to other imaging tests, such as CAT and bone scintigraphy.7
The medical literature has reported good results with MRWS in infants up to a year of corrected gestational age. The procedures took advantage of the postprandial state of infants (the “feed-and-sleep” technique) and the beneficial effect of swaddling; most of them also used an immobilisation system and others used additional strategies, like familiarising the infant with the noise of the MRI machine.11 In NBs, exposure to noise with this purpose may not be justified given the deleterious effects that noise can have in this period of life. The development of immobilisation systems appropriate for this age group and other techniques12 may improve our ability to perform imaging tests without sedation in increasingly older ages.
Thus, while there are still few published studies, the existing ones report very satisfactory experiences in performing imaging tests (MRI, CAT and others) without sedation or anaesthesia, reducing the risks to the child. The results obtained in our study are consistent with what is reported in the literature. We showed that it is possible to perform MRWS in our setting, doing most of the preparation in the neonatal unit to reduce the total time spent in the MRI room. Magnetic resonance without sedation opens the doors to new indications for MRI in NBs and young infants, and facilitates the use of MRI in research studies.
Conflicts of interestThe authors have no conflicts of interest to declare.
We want to thank the health care professionals of the neonatology unit of the Erasmus Medical Centre-Sophia of Rotterdam, and especially Annemarie Plaisier, Marlou M.A. Raets, Paul Govaert and Jeroen Dudink for their hospitality and generosity in sharing their knowledge in a selfless manner.
Please cite this article as: Ureta-Velasco N, Martínez-de Aragón A, Moral-Pumarega MT, Núñez-Enamorado N, Bergón-Sendín E, Pallás-Alonso CR. Resonancia magnética sin sedación en recién nacidos. An Pediatr (Barc). 2015;82:354–359.
Previous presentation: this study was presented as a poster at the XXIV Congreso de Neonatología y Medicina Perinatal and IV Congreso de Enfermería Neonatal, October 2–4, 2013, Barcelona, Spain