A medical visit for plant ingestion is rare in the paediatric emergency services but may involve a high toxicity. The botanical toxicology training of health staff is often very limited, and it can be difficult to make a diagnosis or decide on the appropriate treatment.
ObjectiveTo study the epidemiological and clinical characteristics of poisoning due to plant ingestion in order to increase the knowledge of the health professional.
Material and methodsA descriptive retrospective study was conducted on patients seen in a paediatric emergency department after the ingestion of plant substances from January 2008 to December 2012.
ResultsDuring the period of study, 18 patients had ingested possible toxic plants. In 14 cases, it was considered to be potentially toxic: broom, oleander, mistletoe, butcher's broom, and vulgar bean (2), Jerusalem tomato, castor (2), Jimson weed, potus, marijuana, and mushrooms with digestive toxicity (2). Among the potentially toxic cases, the ingestion was accidental in 10 patients, 2 cases were classed as child abuse, 1 case had recreational intention, and another one suicidal intentions. The ingestion of oleander, castor and Jimson weed had major toxicity.
ConclusionsThe potential gravity of the ingestion of plant substances and the variety of the exposure mechanism requires the paediatrician to bear in mind this possibility, and to be prepared for its diagnosis and management. Specific preventive information measures need to be designed for the families and for the regulation of toxic plants in playgrounds.
La consulta por ingesta de plantas es poco habitual en los Servicios de Urgencias pediátricas pero puede conllevar una elevada toxicidad. La formación sobre toxicología botánica del personal sanitario suele ser escasa y puede resultar difícil llegar al diagnóstico o establecer el tratamiento adecuado.
ObjetivoEstudiar las características epidemiológicas y clínicas de las intoxicaciones por ingesta de sustancias vegetales con el fin de aumentar su conocimiento en el personal sanitario.
Materiales y métodosEstudio descriptivo retrospectivo de los pacientes atendidos por ingesta de sustancia vegetal, entre enero del 2008 y diciembre del 2012, en el Servicio de Urgencias de un hospital materno-infantil de tercer nivel.
ResultadosDurante el periodo de estudio fueron atendidos 18 pacientes con ingesta de un posible tóxico vegetal. En 14 casos la ingesta se consideró potencialmente tóxica: retama, adelfa, muérdago, acebillo, judía vulgar (2), tomate de Jerusalén, ricino (2), estramonio, potus, marihuana y setas con toxicidad digestiva (2). De estos, en 10 la ingesta fue no intencionada, 2 casos pueden enmarcarse en el maltrato infantil, se produjo un caso con fin recreativo y otro con fin suicida. Destacaron por su toxicidad las ingestas de adelfa, ricino y estramonio.
ConclusionesLa potencial gravedad de la ingesta de sustancias vegetales y la variedad de los mecanismos de exposición al tóxico obligan al pediatra a tener presente esta posibilidad y estar preparado para su diagnóstico y manejo. Es necesario diseñar medidas preventivas específicas, como la información a las familias o la regulación de la presencia de plantas tóxicas en zonas de recreo.
For millennia, man has used plants with ornamental, medicinal and recreational purposes. The most ancient poisons also come from plants. We must not forget that many members of the plant kingdom have toxins that can be highly poisonous, even lethal, if ingested.
At present, despite the development and implementation of toxicology surveillance systems, poisoning by ingestion of plant substances continues to be a preventable cause of morbidity and mortality.1
The Poison Control Centers (PCCs) of the United States reported over 30 000 potential exposures to toxic plants in children younger than 5 years in 2012, accounting for 2.8% of medical consultations in this age group, with toxic plants constituting the ninth most frequent substance category involved in paediatric exposures.2 Recent studies in some European countries, like Germany, show a much higher prevalence of up to one-third of all toxic exposures in this age group.3 In Spain, the Servicio Nacional de Información Toxicológica (National Service of Toxicological Information [SIT]) received approximately 500 phone calls for exposures to presumed poisonous plants (0.5% of the total volume).4 However, most cases of exposure in Spain do not result in calls to the SIT, so it is difficult to assess the actual prevalence of plant poisoning.
The exploratory behaviours and the limited risk perception characteristic of children are the reason for the higher incidence in this population. Thus, as the literature describes, up to 85% of plant poisoning cases involve children, especially younger than 5 years.1,3 For the same reason, the main exposure mechanism in children is unintentional.5 However, the possibility of voluntary exposure with suicidal or recreational intent and of poisoning in the context of child abuse must also be considered.5,6
Arriving at the correct diagnosis is particularly difficult in this type of poisoning, so they are probably underdiagnosed. Part of the reason for this is that often neither the patient nor the family associates the symptoms with exposure to a plant, and sometimes the exposure was not even witnessed by the adults. The correlation between taxonomy and toxicology is also poor, as members of the same plant family can cause different clinical manifestations.7,8 This is compounded by the fact that the paediatrician frequently lacks the botanical knowledge required to guide the differential diagnosis.
The aim of this study was to study the epidemiological and clinical characteristics of cases of poisoning by ingestion of plant substances in a paediatric emergency department to determine their prevalence and to expand the knowledge of health care providers on this subject.
Materials and methodsWe conducted a retrospective descriptive study between January 2008 and December 2012 in the emergency department of an urban tertiary maternity and children's hospital, which received a mean 92 000 patient visits a year during the period under study.
Patients were selected by the retrospective review of the electronic medical records of all patients in whom the reason for the visit or the final diagnosis involved poison exposure. Out of the total, we selected the patients 0–18 years of age with suspected poisoning following ingestion of a plant material. The identification of the plants involved was mostly done by the health care staff of the emergency department with the help of a sample provided by the family and/or by the visual recognition of the plant in reference books and web pages on the subject of botany.9–11 A mycologist was consulted in cases of mushroom ingestion and was responsible for identifying the species.
We assessed the potential toxicity of the ingestion based on the presence of symptoms or on the intrinsic toxicity of the plant involved.
We collected data for epidemiological, clinical, and treatment variables.
The data collected for the study were stored and processed in a Microsoft Access relational database created for the purpose. We analysed quantitative and categorical variables, and performed a statistical description of the sample by means of medians and ranges for quantitative variables and frequencies and percentages for categorical ones.
ResultsDuring the period under study, 1885 patients sought services in the emergency department for suspected poisoning (0.4% of the total number of visits). Among them, 18 cases (1%) involved the ingestion of a possibly toxic plant. In 14 cases the ingestion was considered potentially toxic either because the plant was known to be poisonous or because there were clinical manifestations suggestive of toxicity. The median age of this group was 4.3 years (IQR, 1.9–13.1) and the sex distribution was homogeneous (7 male and 7 female patients).
The plant materials involved in these cases were Spanish broom flowers, oleander flowers, mistletoe berries, butcher's broom berries, common bean fruits, Jerusalem cherry fruits, castor oil plant seeds, jimson weed seeds, golden pothos leaves, marihuana leaves, and poisonous mushrooms. Of all of the above, the potentially lethal plants are oleander and the seeds of the castor oil plant.
The mechanism of exposure was unintentional in 10 cases. One adolescent drank a jimson weed infusion for recreational purposes, another attempted suicide by ingesting oleander flowers, and two girls ingested a cake that contained marihuana with the knowledge of the adults responsible for them, which met the criteria for child abuse.
Eleven patients had symptoms, of which vomiting was the most frequent (7 cases). The most severe cases corresponded to ingestion of oleander (Nerium oleander) and of jimson weed (Datura stramonium).
Seven patients were discharged home with no need for observation or supportive therapy due to the low toxicity of the ingested substance (4 cases) or to the time elapsed since ingestion and the absence of toxicity at the time of the assessment (3 cases). Four were kept under observation for a few hours, and seven required admission, one of them to the intensive care unit. When it came to specific treatment for poisoning, activated charcoal was given to one patient for gastrointestinal decontamination, and antidotes were given to none. All patients had good outcomes.
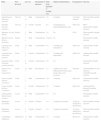
Table 1 shows the main characteristics of patients that had ingested potentially toxic plant substances.
Clinical characteristics of cases of ingestion of a potentially toxic plant.
| Plant | Part involved | Age | Sex | Mechanism of exposure | Time from ingestion to seeking care | Clinical manifestations | Management | Outcome |
|---|---|---|---|---|---|---|---|---|
| Spanish broom (Spartium junceum) | Flowers | 7 m | Male | Unintentional | 2h | Vomiting | Activated charcoal | ObservationFavourable outcome |
| Oleander (Nerium oleander) | Flowers | 15 y | Female | Suicidal | 6h | VomitingSensory abnormalitiesBradycardia | Blood test | PICU admissionFavourable outcome |
| Mistletoe (Viscum album) | Berries | 2 y | Male | Unintentional | 2h | No | ECG | ObservationFavourable outcome |
| Butcher's broom (Ruscus aculeatus) | Berries | 7 y | Male | Unintentional | Unclear | No | DischargeFavourable outcome | |
| Common bean (Phaseolus vulgaris) | Fruits | 13 y | Male | Unintentional | 4h | Vomiting and dehydration | Blood test | AdmissionFavourable outcome |
| Common bean (Phaseolus vulgaris) | Fruits | 4 y | Female | Unintentional | 4h | Vomiting and dehydration | Blood test | AdmissionFavourable outcome |
| Jerusalem cherry (Solanum pseudocapsicum) | Fruits | 8 m | Female | Unintentional | 2h | No | DischargeFavourable outcome | |
| Jimson weed (Datura stramonium) | Seeds | 16 y | Male | Recreational | 3h | Agitation and visual hallucinationsTachycardia, facial redness and mydriasis | Restraint | AdmissionPhysical and chemical restraintFavourable outcome |
| Castor oil plant (Ricinus communis) | Seeds | 2 y | Male | Unintentional | 18h | Vomiting | Blood test | AdmissionFavourable outcome |
| Castor oil plant (Ricinus communis) | Seeds | 2 y | Female | Unintentional | 3h | Vomiting | Blood test | AdmissionFluid therapyFavourable outcome |
| Golden pothos (Epipremnum aureum) | Leaves | 10 m | Male | Unintentional | 6h | No | DischargeFavourable outcome | |
| Marihuana (Cannabis) | Leaves | 11 y | Female | Criminal | 3h | Conjunctival injection | Toxins in urineCall to the DGAIA | ObservationFavourable outcome |
| Marihuana (Cannabis) | Leaves | 4 y | Female | Criminal | 3h | Conjunctival injection | Toxins in urineCall to the DGAIA | ObservationFavourable outcome |
| Unidentified mushroom | Mushrooms | 13 y | Male | Unintentional | 7h | Vomiting | Blood test | AdmissionFavourable outcome |
The DGAIA is a Catalonian institution that promotes the well-being of children and adolescents at high risk for social marginalisation.
DGAIA, Dirección General de Atención a la Infancia y Adolescencia; h, hours; m, months meses; PICU, paediatric intensive care unit; y, years.
The ingestion of toxic plant substances, while rare in comparison to other sources of poisoning, can cause a wide range of clinical manifestations that may be severe,1,3,6 as evinced by the data we present.
Although the number of cases registered in the PCCs of the United States suggests that their incidence has been decreasing in recent decades,2 it is believed that it may be underestimated because cases of plant poisoning may not be properly identified, and some of them may be classified as exposures to an unknown poison.2,6,12
Studies performed in the United States with information from the database of the PCCs, like the one by Carter and Neuspiel, show that most patients exposed to a potentially toxic plant either did not experience poisoning or experienced mild toxicity. In that study, 10% of exposed individuals that consulted with a PCC required medical care.12 However, our series had a higher percentage of patients with clinical symptoms, possibly because, unlike the cases in the study by Carter and Neuspiel, these cases corresponded to patients that ingested toxic plants accidentally and sought care at a hospital emergency department.
The expected toxicity of ingested toxic plants depends on various factors. Some depend on the plant (type, growth and maturation, part ingested, and amount), while others depend on the patient (weight, age) or the time elapsed since ingestion.
When it comes to age, the most frequent mechanism of exposure to toxic plants in the early years of life is unintentional,3 although poisoning can also occur in the context of child abuse or the use of plant materials for medicinal purposes. However, the highest rates of morbidity and mortality are found in children from 13 to 18 years,6 in whom recreational and suicidal intent are most prevalent. As observed in our series, severe poisoning occurs in intentional exposures, while the rest of the cases usually involve the ingestion of small amounts and mild symptoms.
According to previous studies, the sex of the patient is another factor associated with the risk of ingestion.3,6 Krenzelok and Mrvos6 reviewed all the cases of plant ingestion that led to a consultation with the PCCs from 1983 to 2009 and found that most cases occurred in males, and that males were involved in more than 60% of moderate and severe cases. In contrast, in our series the ingestion of potentially lethal plants (oleander and castor oil plant) occurred in female patients, and the distribution of all patients by sex was homogeneous, which may be partly due to the small size of our sample and the low severity of most cases.
Studies conducted in different Spanish hospitals5,7,13–15 had results similar to ours in terms of the epidemiology and the clinical manifestations of cases of poisoning by ingestion of toxic plants. Most cases occur in children younger than 5 years and result from unintentional exposure. Mild gastrointestinal symptoms are the most common presentation. The plants implicated most frequently are Ricinus communis, N. oleander and D. stramonium, and Robinia pseudoacacia, which was not found in our study, is often mentioned in others. In 1983, García et al. described a series of 25 cases of unintentional poisoning by redoul (Coriaria myrtifolia) in Catalonia, with the development of florid symptoms that ranged from gastrointestinal involvement to severe neurological effects, including convulsions, agitation and even coma.15C. myrtifolia abounds in Mediterranean mountains, but there were no cases of exposure to it in our series.
In the reports of the American Association of Poison Control Centers (AAPCC), the specific species involved in most cases of exposure to toxic plants is unknown. The most frequent among the known plants were those that cause gastrointestinal symptoms, such as Dieffenbachia in the Araceae family. This family is comprised of several ornamental plants that contain toxic oxalate crystals. When these crystals come into contact with the oral mucosa they cause severe oedema and pain. There were no cases of Dieffenbachia exposure, but there were cases involving golden pothos (Epipremnum aureum), which belongs to the same family. Poisonings by D. stramonium are also frequent, especially in regions like Central America, and the plant causes a considerable number of cases with moderate and severe symptoms.3,16
As for severity, the study of Krenzelock and Mrvos found that plants in the Cicuta (with a curare-like effect) and the Datura families caused more than one-third of the deaths by ingestion of toxic plants in the United States.6 While no fatalities have been reported in Spain, most potentially lethal cases are associated with plants in the Cicuta family (which resemble parsley) and, as observed in our case series, N. oleander and R. communis.5,14
As described in the literature and observed in the cases presented here, the treatment of most cases of plant poisoning is based on symptom management, and starts with stabilising the patient (ABC approach).1,6,8,9,12 Theoretically, gastrointestinal decontamination by activated charcoal can be used to minimise absorption of plant toxins, but the clinical characteristics of these poisonings prevent this method from being particularly useful overall and in clinical practise: poisoning is usually suspected only after symptoms develop, so that there is a long delay from ingestion to seeking care, and the predominant presentation of vomiting induces the spontaneous emptying of gastric contents. Administration of antidotes as specific therapy could be indicated on rare occasions of poisoning by plants containing digitalis glycosides or anticholinergic agents.8,9 This applies to poisoning by N. oleander and D. stramonium. All parts of the former contain cardiac glycosides similar to digoxin that cause digitalis poisoning, which is potentially lethal due to cardiac involvement. Administration of specific antibodies against digoxin Fab fragments can be used to reverse cardiac toxicity and is indicated in cases with evidence of hyperkalaemia or ventricular arrhythmias. The D. stramonium plant contains tropane alkaloids that have peripheral and central anticholinergic effects. The presence of severe central anticholinergic toxicity is an indication for the administration of physostigmine to reverse the symptoms, although this medication must be used with caution and while monitoring the patient due to its significant cardiovascular side effects.9 Similar to what has been described in other studies, most cases of poisoning presented in this series were managed with supportive therapy alone.6,8,9,12 Knowing which plants are candidates for antidote treatment is important, but most of the described cases of poisoning by digitalis glycosides or anticholinergic agents had good outcomes after admission to the hospital with careful monitoring and symptomatic treatment alone.8,12,14
Overall, the general population has little knowledge of the toxicity of plants present in their environment. In most cases described in this study, the plant was identified by toxicology tests performed by clinicians, and parents only knew that the involved plant was toxic in four cases. It is also frequent for paediatricians to experience great difficulty identifying the responsible plant and determining its expected toxicity due to their limited knowledge of plants. Thus, it is useful to know the most common toxic plants in the area, how to use online resources for their correct identification, and the basic elements in the management of poisoning by these plants.9–11
Table 2 describes the main botanical characteristics of the most common toxic plants in Spain, which may be used as an aid in the identification of plants by health care professionals.1,4,10,11,14
Botanical characteristics of the plants most frequently involved in poisoning by ingestion.
| Name | Morphology | Toxic product | Habitat | Main symptoms | |
|---|---|---|---|---|---|
| Mistletoe (Viscum album) | Berries | Small green berries that later become clear, white or yellowish. Yellow–green lanceolate leaves | Whole plant | Parasite of other treesCold and temperate climates | Gastrointestinal |
| Redoul (Coriaria myrtifolia) | Berries | Shrub with berries that are first red and then black | Whole plant | Streams and edges of woods | CNS stimulant |
| Belladona (Atropa belladona) | Berries | Branching subshrub with long oval leaves and purple bell-shaped flowersBlack round berries | Whole plant | Shady woodsCold climatesElevationsCalcareous soils | Atropine syndrome |
| Jerusalem cherry (Solanum pseudocapsicum) | Berries | Berries like small bright red tomatoes, resembling cherries | Berries | Ornamental | Cholinergic |
| Butcher's broom (Ruscus aculeatus) | Berries | Small dark-green shrub with small leaves and greenish or purplish flowersRed round berries | Berries | ParksShady woodsCold climates | Gastrointestinal |
| Castor oil plant (Ricinus communis) | No berries | Thick woody shrub with large dark purple leavesLarge, smooth, mottled, shiny oval seeds of a red-brown colour | Seeds | Gardens and parksOrnamental | Gastrointestinal |
| Common bean (Phaseolus vulgaris) | Without berries | Raw seeds and green beans | Seeds and beans | Farmland | Gastrointestinal |
| Hemlock (Conium maculatum) | Without berries | Plant resembling parsley or fennel but darker and with an unpleasant odour. Brown–green oval fruits | Fruits | Edges of roads | Neuromuscular paralysis |
| Dumb cane (Dieffenbachia) | Without berries | Tall plant with a straight stem and dark green oval leaves with light specks | Whole plant | Tropical ornamental plant | Oropharyngeal irritationGastrointestinal |
| Golden pothos (Epipremnum aureum) | Without berries | Thick-stemmed vine with showy heart-shaped green and yellow leaves | Foliage | Tropical ornamental plant | Oropharyngeal irritationGastrointestinal |
| Jimson weed (Datura stramonium) | Without berries | Herb with erect fruits in spiny capsules | Whole plant | Vacant lotsRoad edgesDumps | Atropine syndrome |
| Oleander (Nerium oleander) | Without berries | Showy shrub with pink flowers that can also be white, yellow and red | Whole plant | Valleys and cliffsGardens | Cardiac |
| Foxglove (Digitalis purpurea) | Without berries | Tubular pink or purple flowers hanging in clusters en | Whole plant | Paths and clearings in humid woodsOrnamental | Cardiac |
| Spanish broom (Spartium junceum) | Without berries | Greenish-grey plant that grows in shrubs with small leavesPlentiful yellow fragrant flowers and black seeds | Flowers | Sunny rocky areasMediterranean climateOrnamental | Cardiovascular |
| Marihuana (Cannabis) | Without berries | Tall light green plant. Dry greenish flower shaped like a feather, long green leaves. Swollen fruits with black seeds | Flowers, foliage and stem | Crops | Psychotropic |
There are limitations to this study. Some data may be missing due to the retrospective design. Thus, we cannot rule out having missed some cases of nontoxic plant ingestion that were not initially classified as a suspected poison exposure. Furthermore, the study did not analyse the potential toxicity or side effects associated to plants ingested for medicinal purposes. Lastly, since it was a single-centre study, it poses challenges to inferring the incidence of poisoning by ingestion of toxic plants. The participation of other emergency departments, especially in rural settings, would complete the data obtained in our study.
To conclude, plants continue to cause poisonings, which in some cases are severe and preventable. In order to prevent plant poisonings, the general population as well as health care providers need to be better informed on the toxicity of plants, and the presence of the highly toxic plants in recreational spaces must be regulated.
Conflict of interestThe authors have no conflicts of interest to declare.
Please cite this article as: Martínez Monseny A, Martínez Sánchez L, Margarit Soler A, Trenchs Sainz de la Maza V, Luaces Cubells C. Tóxicos vegetales: un problema aún vigente. An Pediatr (Barc). 2015;82:347–353.
Previous presentation: partial results of this study were presented as oral communications at the XVIII Reunión de la Sociedad Española de Urgencias Pediátricas, April 2013, Granada, Spain.