The mortality of children with a birthweight of less than 1500g or with a gestational age of less than 32 weeks (<1500<32) has decreased significantly in the last 20 years or so. Given the higher risk of disability in these children, follow-up after hospital discharge is considered essential. In this document, the Follow-Up Group of the Spanish Society of Neonatology, in collaboration with the Spanish Society of Paediatric Primary Care, propose a follow-up protocol specific for the <1500<32, which has as its aim to standardise the activities and evaluations according to good practice criteria.
La mortalidad de los niños nacidos con peso menor de 1.500g o con una edad gestacional menor de 32 semanas (<1.500<32) ha disminuido significativamente en las últimas décadas. Dado el mayor riesgo de discapacidad de estos niños, el seguimiento tras el alta hospitalaria se considera muy necesario. En este documento, el Grupo de Seguimiento de la Sociedad Española de Neonatología, en colaboración con la Asociación Española de Pediatría de Atención Primaria, propone un protocolo de seguimiento específico para los<1.500<32, cuyo objetivo es estandarizar las actividades y evaluaciones según los criterios de buena práctica.
The advances made in neonatal care in recent decades have succeeded in significantly reducing mortality in infants with very low birth weight (VLBW<1500g) or born very preterm (VPT<32 weeks’ gestation). Given the increased risk of future disability in VLBW/VPT children, their followup after discharge is considered a crucial component of neonatal care. In some countries, the development of a follow-up programme is an essential prerequisite for hospitals to gain accreditation to train specialists in neonatology.1 However, it is also known that generally speaking, countries do not have established clinical guidelines or consensus protocols of national scope that allowing the standardised followup of these children.1–4
It is generally believed that followup should continue until at least 2 years of corrected age (CA). However, it is also assumed that this timeframe mainly results in the detection of moderate to severe disability, while much of the morbidity that develops at a later time in these children, which usually involves emotion, behaviour and learning, goes undetected and untreated. Thus, follow-up programmes would ideally extend to age 5–7 years or even through adolescence.4
For all the reasons noted above, and given that there currently are no follow-up protocols for VLBW/VPT children of national scope, the Sociedad Española de Neonatología (Spanish Society of Neonatology), in collaboration with the Asociación Española de Pediatría de Atención Primaria (Spanish Association of Primary Care Paediatrics), proposes a specific protocol for the followup of VLBW/VPT infants, understood as a guideline of general interventions for standardising the care of these children based on good clinical practice criteria.
The needs of VLBW/VPT children during the followup years are very diverse and often complex. This protocol focuses on aspects applicable to the followup of all these children, regardless of the setting where they are evaluated. Needless to say, other services that are not included in this protocol will have to be provided based on the specific problems experienced by each child and family.
The objectives in developing this protocol were:
- •
To establish and standardise the follow-up evaluations that must be performed in VLBW/VPT children, including evidence-based practices to the extent possible.
- •
To promote the coordination of services offered at the primary care (PC) level and in hospital-based follow-up clinics.
- •
To provide helpful guidance to clinicians responsible for the care of VLBW/VPT children.
- •
To define a series of simple indicators to assess the degree to which different facilities and autonomous communities in Spain adhere to the protocol, with the ultimate goal of ensuring that all children have equal access to health care resources.
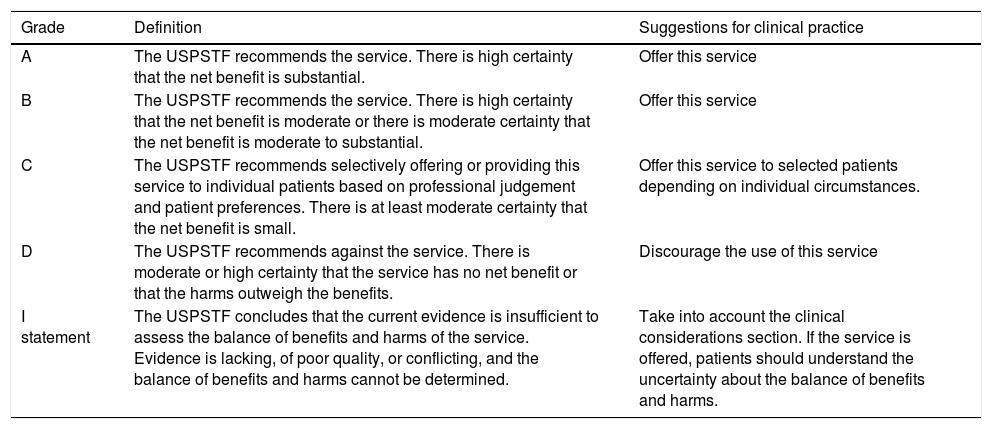
The Sociedad Española de Neonatología recommends the inclusion of all infants born with a weight of less than 1500g or before 32 weeks’ gestation in a standardised follow-up programme until at least school age (6–7 years). The development of follow-up programmes in collaboration with other professionals is an essential element in the activity of level III neonatal care units.1,5,6 Grade B recommendation. Table 1 presents the definitions for the different grades of recommendation.7
Grade definitions of the USPSTF.7
| Grade | Definition | Suggestions for clinical practice |
|---|---|---|
| A | The USPSTF recommends the service. There is high certainty that the net benefit is substantial. | Offer this service |
| B | The USPSTF recommends the service. There is high certainty that the net benefit is moderate or there is moderate certainty that the net benefit is moderate to substantial. | Offer this service |
| C | The USPSTF recommends selectively offering or providing this service to individual patients based on professional judgement and patient preferences. There is at least moderate certainty that the net benefit is small. | Offer this service to selected patients depending on individual circumstances. |
| D | The USPSTF recommends against the service. There is moderate or high certainty that the service has no net benefit or that the harms outweigh the benefits. | Discourage the use of this service |
| I statement | The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of the service. Evidence is lacking, of poor quality, or conflicting, and the balance of benefits and harms cannot be determined. | Take into account the clinical considerations section. If the service is offered, patients should understand the uncertainty about the balance of benefits and harms. |
For this article, we used the Spanish translation featured in the following working manual of the PrevInfad group: http://previnfad.aepap.org/manual-de-trabajo#9.5. We received authorisation for its reproduction.
- •
We recommend implementation of the elements of the VLBW/VPT follow-up programme that correspond to the PC level, which will be detailed throughout this document.5 Grade B recommendation.
- •
We recommend the design of strategies at the PC level for the prevention of follow-up dropouts.8–11 Grade B recommendation.
- •
We recommend the development of a continuing education strategy to ensure the appropriate implementation of the follow-up programme at the PC level.5,12 Grade B recommendation.
- •
We recommend that the first PC visit be scheduled before hospital discharge, and that the discharge summary is made available to the paediatrician prior to this visit.13 I statement.
- •
In regard to the Child Health Record booklet, we recommend, in addition to filling out the pertinent data though discharge, attaching the slips displaying the lots of any administered vaccines, and writing down the record number for the newborn screening test and the results of the hearing screen. I statement.
- •
In regard to electronic health records, we recommend for professionals involved in the care of the child (hospital, primary care, early intervention centre) to have access to the different health record databases. This aspect is key for the purpose of coordinating care resources, avoid duplication of records, increasing efficiency and effectiveness, responding quickly to the needs of the infant and the family and retrieving data for assessment of clinical practice or other research purposes. I statement.
- •
We recommend that all VLBW/VPT infants be evaluated by the PC paediatrician within a maximum of 5 days from hospital discharge.14 Grade B recommendation. To achieve this, we advise applying for the child's public health care card and assigning a PC paediatrician and nurse prior to discharge.
- •
In cases of social or environmental risk, we recommend that the PC team ensures that social services are involved and the coordination of care between both settings. I statement.
- •
We recommend monitoring growth from the time of discharge. Reduced growth is associated with poorer neurodevelopmental outcomes. Excessive weight gain is associated with an increased risk of obesity, cardiovascular disease and diabetes in adulthood.15–21 The recommended target for weight gain is 25–35g/day in the first 3 months after discharge. Grade B recommendation.
- •
To assess growth post discharge, we recommend using the revised Fenton preterm growth charts up to 44 weeks’ CA, followed by the World Health Organization (WHO) child growth standards applied to the CA.22,23 I statement.
- •
We recommend that children born small for gestational age whose height is more than 2 standard deviations below the mean in the WHO growth charts at age 2 or 3 years be referred to endocrinology for evaluation and consideration of growth hormone therapy.24 Grade B recommendation.
- •
We recommend exclusive breastfeeding until age 6 months, followed by breastfeeding combined with other foods until age 2 years or the mother and child choose to wean.26 There is evidence that nutrition with human milk is associated with a reduced morbidity during the hospital stay27–30 and better cognitive outcomes.31,32 There are no studies on the benefits of human milk after discharge in this specific group of children. Grade B recommendation.
- •
Since the composition of human milk is highly variable, the volume of milk a child requires to achieve an adequate energy intake also varies. For this reason, we recommend that in children at nutritional risk (who are below the 10th percentile at discharge, under fluid restriction, whose weight gain with exclusive breastfeeding is inadequate or with osteopaenia of prematurity), human milk be fortified with supplements or replaced by preterm formula in some of the feeds (always after verifying that breastfeeding technique is actually correct). There is no evidence of differences in outcome based on the use of fortification versus preterm formula.33–35 I statement.
- •
The most widely recommended approach to fortification of human milk in breastfeeding infants is diluting 4 or 5g of fortifier (depending on the manufacturer) in 30–50mL of expressed breast milk and administering this mixture to the child before breastfeeding 2–3 times a day.36 No other supplements, such as vitamins or iron, should be added to fortified milk. We discourage administration of more than 15g of fortifier a day, as it carries a risk of hypervitaminosis A. The dosage of vitamin D must be adjusted while the child is fed with fortified milk. I statement.
- •
Milk production in the first weeks after discharge can increase by using the kangaroo care approach at home, so we recommend ensuring that all mothers know how to hold the baby in this position before discharge. Numerous studies have evinced the positive effects of kangaroo care in milk production, although most of them were conducted in hospital settings.37,38 Grade B recommendation.
- •
There is considerable controversy regarding the use of enriched standard formula (65kcal/dL) versus preterm formula (75–80kcal/dL) after discharge.39–41 The European Society for Paediatric Gastroenterology Hepatology and Nutrition (ESPGHAN) recommends the use of preterm formula until 40 weeks of postmenstrual age and possibly longer if growth is inadequate.42 The WHO recommends its use only until a weight of 2000g is achieved.43 We cannot make any recommendations on this subject. If the infant is exclusively fed with preterm formula past 40 weeks’ postmenstrual age, attempts should be made to transition from it as soon as possible, as it contributes excessive amounts of phosphorus and calcium.44 However, it may be appropriate to substitute preterm formula in some of the feeds beyond 40 weeks’ postmenstrual age in infants who are breastfeeding or fed standard newborn formula for the purpose of increasing energy intake. I statement.
- •
Complementary foods must be introduced taking into account the motor skills of the child in relation to feeding.45,46 There are no studies demonstrating the advantages or disadvantages of basing the introduction of complementary foods on chronological age versus corrected age, so this process should be individualised in each child. I statement.
- •
Even if motor development seems adequate, we recommend performance of 2 thorough neuromotor evaluations by a specialist in the first year of life.1 Three months of corrected age is a good time for implementation of the Prechtl general movements assessment, which is a strong predictor of future motor function.47,48 This assessment helps identify children likely to have motor impairment in the future so that they can be referred to physical therapy, as they are the children who benefit most from early intervention. The second evaluation can be performed at around 12 months’ CA. Grade B recommendation.
- •
All VLBW/VPT children are at increased risk of motor impairment, so we recommend referral to early intervention services, which have been proven to improve cognitive and motor function outcomes.49,50 Grade A recommendation.
- •
We recommend describing impairments in motor function and skills, when applicable, by means of the various scales available for this purpose. This allows the objective assessment of motor outcomes in the child, and also facilitates comparisons between centres, as it increases uniformity in patient classification.
- •
Use of the kangaroo care method during the hospital stay and after discharge is associated with a reduction in emotional problems and improved stress regulation in school-aged children, yet another reason to recommend its practice in these infants during the hospital stay and after discharge.51,52 Grade A recommendation.
- •
We recommend referral of VLBW/VPT children to early intervention services, as there is evidence that they improve cognitive and motor outcomes.50,53 Grade A recommendation.
- •
We recommend screening every VLBW/VPT child for autism spectrum disorder and other developmental disorders using the M-CHAT scale between 18 and 24 months of CA. If the screen is positive, the child should be referred to a specialist for a formal evaluation Grade B recommendation.
- •
We recommend evaluating behaviour, attention and emotional problems, as these are aspects that could improve with appropriate guidance and treatment. It is important for health providers to be aware of the prevalence of these problems in order to promote their assessment and to offer parents prognostic information regarding every area of development in their child.54,55 Grade B recommendation.
- •
We recommend that the follow-up team include psychologists with the necessary qualifications to perform evaluations and provide counselling and treatment for any problems detected in the child as well as support to the families.54,55 Grade C recommendation.
- •
We recommend performing, at minimum, the Bayley-III test at around 2 years of CA to be able to counsel the child and family and for assessment of outcomes in the group of managed VLBW/VPT infants. This is the scale used by most groups that follow up preterm children.56,57 I statement.
- •
We recommend that PC providers confirm that the infant has been screened for retinopathy of prematurity. If screening has not been performed or completed, the child should be referred an ophthalmologist with experience in screening for retinopathy of prematurity. There is evidence that screening for retinopathy and treating detected cases reduces the incidence of blindness.58,59 Grade A recommendation.
- •
We recommend evaluation of all VLBW/VPT children by an ophthalmologist before age 3 years, as early treatment of amblyopia is associated with improved outomes.60–62 The PC team will confirm that this ophthalmological evaluation has taken place. Grade B recommendation.
- •
Children with stage 3 retinopathy of prematurity, who have required treatment or with neurological deficits require specialised ophthalmological follow-up until adolescence.49,60,63 Primary care paediatricians should verify that these assessments are taking place. Grade B recommendation.
- •
We also recommend that PC paediatricians conduct a screening for vision problems (amblyopia, strabismus and refraction errors) at age 4 or 5 years.64 Grade B recommendation.
- •
We recommend referring the child to the ophthalmologist for an additional evaluation if any abnormality is detected by the paediatrician or reported by the parents.62,65 Grade B recommendation.
- •
We recommend that all VLBW/VPT infants undergo a hearing screen using automated auditory brainstem response or brainstem auditory evoked potential tests before discharge from the neonatal unit.66–69 Primary care paediatricians need to confirm that the hearing screen has been performed. Grade B recommendation.
- •
We recommend performance of an age-appropriate behavioural hearing test at around age 2 years to detect late-onset hearing loss.66–68 Primary care professionals will ensure that testing has been performed. Grade B recommendation.
- •
We recommend referring any child with language problems or whose parents report concerns about the child's hearing for an audiology assessment. Grade B recommendation.
- •
We recommend vitamin D supplementation in preterm infants at a dose of 400IU/day until 1 year of CA.70–72 Grade A recommendation.
- •
Children at higher risk of vitamin D deficiency (treated with loop diuretics, under fluid restriction, under long-term corticosteroid therapy, or fed with hydrolysed formula) may be given up to 1000IU/day.70–72 I statement.
- •
We recommend iron supplementation of breastfed VLBW/VPT infants with 4mg/kg/day (to a maximum of 15mg/day) of ferrous sulfate from 1 month to 1 year of chronological age or until complementary foods contribute a sufficient amount of iron.22,73,74 Grade B recommendation.
- •
For infants fed with preterm, starter infant or follow-up formulas, we recommend iron supplementation with 1.5mg/kg/day of iron sulfate until 1 year of chronological age or until complementary foods contribute a sufficient amount of iron.22,73,74 Grade B recommendation.
- •
We recommend strict adherence to the general recommendations for prevention of respiratory tract infection: breastfeeding, vaccination against influenza of close contacts, adequate hand hygiene and cough etiquette, avoiding exposure to tobacco smoke, and not enrolling the child in a day care centre in the first winter of life. Grade A recommendation.
- •
Generally speaking, VLBW/VPT children should be vaccinated at the same chronological age and with the same schedule and dosage as their peers, regardless of gestational age or weight at birth.75,76 Grade A recommendation.
- •
We recommend avoiding delays in vaccination to achieve and maintain protective levels of antibodies in the early months of life, which is when children are at highest risk of infection.75,76 I statement.
- •
We recommend vaccinating all VLBW/VPT children against influenza every year. For infants of less than 6 months of chronological age, we recommend not vaccinating the child and vaccinating close contacts instead.75,76 Grade B recommendation.
- •
Children born before 32 weeks’ gestation or with birth weights of less than 1700g are at higher risk of invasive infection by Streptococcus pneumonia compared to those born to term, so in these children, vaccination with a 3+1 series of PCV-13 vaccine is particularly recommended, without later administration of the 23-valent polysaccharide vaccine (PPSV-23) unless there are other risk factors.77 Grade B recommendation.
- •
We recommend that any health care workers who come in contact with preterm infants and have not been vaccinated with the tetanus toxoid, reduced diphtheria toxoid and acellular pertussis vaccine (Tdap) be given a dose of it at least 4 weeks apart from the latest received dose of adult tetanus and diphtheria vaccine (Td).78 I statement.
- •
It is important to promote the cocooning strategy, vaccinating all close contacts and caregivers of preterm infants, both in the household and in neonatal care units.79,80 I statement.
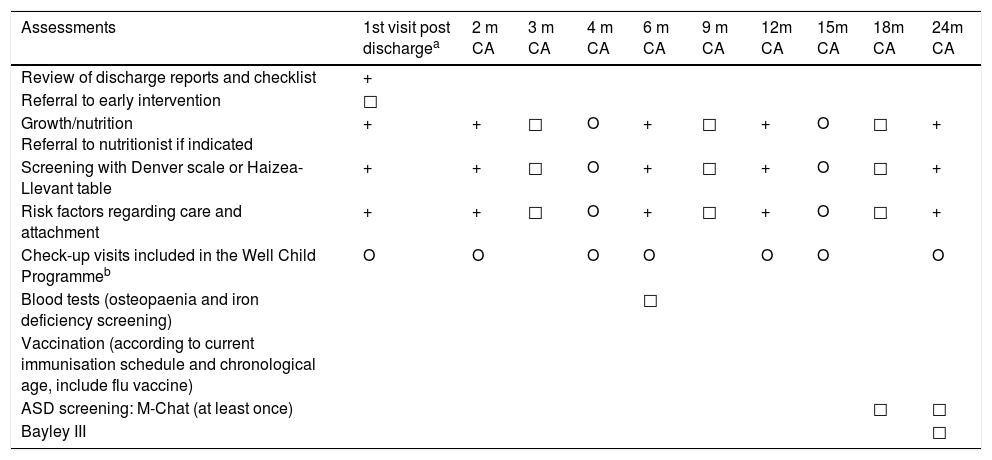
Tables 2–4 show the proposed schedule for follow-up visits.
Hospital and Primary Care followup from discharge to 24 months’ corrected age.
| Assessments | 1st visit post dischargea | 2 m CA | 3 m CA | 4 m CA | 6 m CA | 9 m CA | 12m CA | 15m CA | 18m CA | 24m CA |
|---|---|---|---|---|---|---|---|---|---|---|
| Review of discharge reports and checklist | + | |||||||||
| Referral to early intervention | □ | |||||||||
| Growth/nutrition Referral to nutritionist if indicated | + | + | □ | O | + | □ | + | O | □ | + |
| Screening with Denver scale or Haizea-Llevant table | + | + | □ | O | + | □ | + | O | □ | + |
| Risk factors regarding care and attachment | + | + | □ | O | + | □ | + | O | □ | + |
| Check-up visits included in the Well Child Programmeb | O | O | O | O | O | O | O | |||
| Blood tests (osteopaenia and iron deficiency screening) | □ | |||||||||
| Vaccination (according to current immunisation schedule and chronological age, include flu vaccine) | ||||||||||
| ASD screening: M-Chat (at least once) | □ | □ | ||||||||
| Bayley III | □ |
+: both settings; □: hospital only; O: Primary Care only; ASD: autism spectrum disorder; CA: corrected age.
Assessment by other specialists.
| Specialist | 1st visit post discharge | 3 m CA | 6 m CA | 9 m CA | 12 m CA | 18 m CA | 24 m CA | 3 years |
|---|---|---|---|---|---|---|---|---|
| Neurologist | ||||||||
| All | ||||||||
| Children at high risk or with neurologic involvement: whenever needed | + | + | ||||||
| Ophthalmologist | ||||||||
| All | + (before age 3 years) | |||||||
| High risk. As needed | ||||||||
| Ear specialist | ||||||||
| All (behavioural hearing test) | + | |||||||
CA, corrected age.
In addition, children with health problems will be referred to the pertinent specialist as often as necessary.
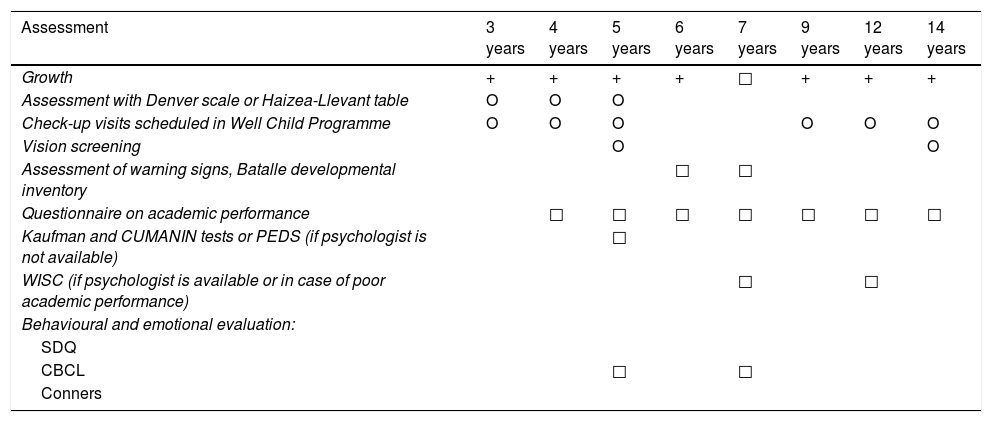
Hospital and Primary Care followup from age 3 to 14 years.
| Assessment | 3 years | 4 years | 5 years | 6 years | 7 years | 9 years | 12 years | 14 years |
|---|---|---|---|---|---|---|---|---|
| Growth | + | + | + | + | □ | + | + | + |
| Assessment with Denver scale or Haizea-Llevant table | O | O | O | |||||
| Check-up visits scheduled in Well Child Programme | O | O | O | O | O | O | ||
| Vision screening | O | O | ||||||
| Assessment of warning signs, Batalle developmental inventory | □ | □ | ||||||
| Questionnaire on academic performance | □ | □ | □ | □ | □ | □ | □ | |
| Kaufman and CUMANIN tests or PEDS (if psychologist is not available) | □ | |||||||
| WISC (if psychologist is available or in case of poor academic performance) | □ | □ | ||||||
| Behavioural and emotional evaluation: | ||||||||
| SDQ | □ | □ | ||||||
| CBCL | ||||||||
| Conners | ||||||||
+: both settings; □: hospital only; O: Primary Care only.
The full text of the protocol is available for download at the website of the Sociedad Española de Neonatología.81
FundingThe meetings for the development of this document and its revision were funded by the Sociedad Española de Neonatología.
Conflict of interestThe authors declare that they have no conflicts of interest.
We want to thank the external reviewers: Thais Agut Quijano (neonatologist), Nuria Boronat González, Julia Colomer Revuelta, Olga Cortés Rico, Javier de la Cruz Bértolo, María Jesús Esparza Olcina, José Galbe Sánchez-Ventura, Jaime García Aguado, José Antonio Hurtado Suazo, María López Maestro (neonatologist), Miriam Martínez Biarge, Ana Martínez Rubio, José Mengual Gil, Manuel Merino Moína, Josep Perapoch López, Javier Sánchez Ruiz-Cabello, Purificación Sierra García, Mónica Vírchez Figueroa.
We also thank the Maternal and Child Health and Development Research Network (SAMID network), funded by the Instituto de Salud Carlos III (RD16/0022/0015) (2017–2021).
Lastly, the Asociación Española de Pediatría de Atención Primaria for its support and participation in the diffusion of this protocol.
Please cite this article as: Pallás Alonso C, García González P, Jimenez Moya A, Loureiro González B, Martín Peinador Y, Soriano Faura J, et al. Protocolo de seguimiento para el recién nacido menor de 1.500 g o menor de 32 semanas de edad gestación. An Pediatr (Barc). 2018;88:229.e1–229.e10.
Previous presentation: This protocol was presented at a round table held at the XXVI Congress of Neonatology and Perinatal Medicine; September 27–29, 2017; Zaragoza, Spain.